 |
 |
| Korean J Med > Volume 96(4); 2021 > Article |
|
Abstract
Endoscopic retrograde cholangiopancreatography (ERCP)-related iatrogenic perforations are identified when gas or luminal contents exit the gastrointestinal tract during ERCP. Although perforations are rare, mortality is high; prompt diagnosis and appropriate management are essential. A multidisciplinary approach is required. The vast majority of such patients can be safely managed medically and endoscopically but must be carefully selected. Endoscopic closure can be considered, depending on the type of perforation. In patients who are deteriorating or whose iatrogenic perforations are not securely closed endoscopically, surgery is mandatory.
ļé┤ņŗ£Ļ▓ĮņĀü ņŚŁĒ¢ēņä▒ ņĘīļŗ┤ļÅä ņĪ░ņśüņłĀ(endoscopic retrograde cholangiopancreatography, ERCP) ņŗ£Ē¢ē ņżæņŚÉ ļ░£ņāØĒĢśļŖö ņØśņØĖņä▒ ņ▓£Ļ│ĄņØĆ ļō£ļ¼╝ņ¦Ćļ¦ī ņŗ¼Ļ░üĒĢ£ ļČĆņ×æņÜ®ņ£╝ļĪ£ ņŗĀņåŹĒĢ£ ņ¦äļŗ©Ļ│╝ ņĀüņĀłĒĢ£ Ļ┤Ćļ”¼Ļ░Ć ļ¦żņÜ░ ņżæņÜöĒĢśļŗż. ņĄ£ĻĘ╝ ņ£Āļ¤Į ņåīĒÖöĻĖ░ļé┤ņŗ£Ļ▓ĮĒśæĒÜī(European Society of Gastrointestinal Endoscopy, ESGE)ņŚÉņä£ ERCP ņŚ░Ļ┤Ć ņ▓£Ļ│ĄņØś ņ▓śņ╣śņÖĆ Ļ┤ĆļĀ©ļÉ£ 2014ļģä ĻČīĻ│ĀņĢłņØä Ļ░£ņĀĢĒĢśņŚ¼ ļ░£Ēæ£ĒĢśņśĆļŗż[1]. ņØśņØĖņä▒ ņ▓£Ļ│ĄņØĆ ļ░£ņāØ ļ╣łļÅäĻ░Ć ļé«ĻĖ░ ļĢīļ¼ĖņŚÉ ļīĆĻĘ£ļ¬©ņØś ņĀäĒ¢ź ņŚ░ĻĄ¼Ļ░Ć ņ¢┤ļĀĄĻ│Ā, ļö░ļØ╝ņä£ ņĄ£ņŗĀ ESGEņØś ĻČīĻ│ĀņĢłļÅä Ļ░ĆņØ┤ļō£ļØ╝ņØĖņØ┤ ņĢäļŗī ņ×ģņן Ēæ£ļ¬ģņ£╝ļĪ£ ņĀ£ĒĢ£ļÉśļŖö ļŗ©ņĀÉņØ┤ ņ׳ļŗż.
ERCP ņŚ░Ļ┤Ć ņ▓£Ļ│ĄņØĆ ņŗ£ņłĀ Ēøä Ļ░ĆņŖż ļśÉļŖö ņןĻ┤Ć ļé┤ņÜ®ļ¼╝ņØ┤ ņ£äņןĻ┤Ć ņÖĖļČĆņŚÉņä£ Ļ┤Ćņ░░ļÉśĻ▒░ļéś, ļśÉļŖö ļé┤ņŗ£Ļ▓Į Ļ▓Ćņé¼ ņżæ ņ£ĪņĢłņ£╝ļĪ£ ņ▓£Ļ│ĄņØ┤ ĒÖĢņØĖļÉ£ Ļ▓ĮņÜ░ļĪ£ ņĀĢņØśĒĢ£ļŗż[2].
ņ▓£Ļ│ĄņØś ņ¦äļŗ© ņŗ£ĻĖ░ļŖö ņ╣śļŻī ļ░Å ĒÖśņ×É ņśłĒøäņŚÉ Ļ▓░ņĀĢņĀüņØĖ ņśüĒ¢źņØä ļ»Ėņ╣£ļŗż[3,4]. ĒÖśņ×ÉĻ░Ć ļ│ĄļČĆ ĒīĮļ¦īņØä ļÅÖļ░śĒĢ£ ļ╣ä ņĀäĒśĢņĀü ļ│ĄĒåĄ, ĒØēĒåĄ, Ēö╝ĒĢś ĻĖ░ņóģ, ĒśĖĒØĪĻ│żļ×ĆņØä ĒśĖņåīĒĢśļ®┤ ņØśņØĖņä▒ ņ▓£Ļ│ĄņØä ņØśņŗ¼ĒĢ┤ņĢ╝ ĒĢśļ®░, ņ¦äļŗ©ņØ┤ ņ¦ĆņŚ░ļÉśļ®┤ systemic inflammatory response syndrome, ņĀĆĒśłņĢĢ, ņĀĢņŗĀņ░®ļ×Ć ļō▒ņØś ņŗ¼Ļ░üĒĢ£ ņ”ØņāüņØ┤ ļ░£ņāØĒĢśĻ▓ī ļÉ£ļŗż. ņ▓£Ļ│ĄņØś ņĪ░ĻĖ░ ņ¦äļŗ©ņØĆ ņן ļé┤ņÜ®ļ¼╝ņØś ļŗżļ¤ē ļłäņČ£ļĪ£ ņØĖĒĢ£ ņśżņŚ╝ņØä ļ░®ņ¦ĆĒĢśņŚ¼ ņłśņłĀ ļ░Å ļé┤ņŗ£Ļ▓Į ņ╣śļŻīļź╝ Ļ░ĆļŖźĒĢśĻ▓ī ĒĢśļ»ĆļĪ£ ņśłĒøäņŚÉ ņżæņÜöĒĢ£ ņśüĒ¢źņØä ļ»Ėņ╣śĻ▓ī ļÉ£ļŗż[5-8]. ņ▓£Ļ│ĄņØś ņśüņāü ņ¦äļŗ©ņØä ņ£äĒĢ┤ ļ│ĄļČĆ ļŗ©ņł£ņ┤¼ņśü, ļ│ĄļČĆ ņĀäņé░ĒÖöļŗ©ņĖĄņ┤¼ņśü(computed tomography, CT) ļō▒ņØ┤ Ļ░Ćņן ļ¦ÄņØ┤ ņé¼ņÜ®ļÉ£ļŗż[9]. ļ│ĄļČĆ CTļŖö ņåīļ¤ēņØś ņןĻ┤Ć ņÖĖ Ļ░ĆņŖż, ņןĻ┤Ć ļé┤ņÜ®ļ¼╝ ļō▒ņØś Ļ░Éņ¦ĆĻ░Ć Ļ░ĆļŖźĒĢśļ®░, ņ▓£Ļ│ĄņŚÉ ļīĆĒĢ£ ļé┤ņŗ£Ļ▓Į ņ╣śļŻī Ēøä ņÖäļ▓ĮĒĢ£ ĒÅÉņćä ņŚ¼ļČĆļÅä ĒÖĢņØĖņØ┤ Ļ░ĆļŖźĒĢśļŗż[6,10]. ņłśņÜ®ņä▒ ņĪ░ņśüņĀ£ ņäŁņĘ© Ēøä ļ│ĄļČĆ CT Ļ▓Ćņé¼ļź╝ ņŗ£Ē¢ēĒĢśļ®┤ ļłäņČ£ ļČĆņ£äĻ░Ć ĒÜ©Ļ│╝ņĀüņ£╝ļĪ£ Ēæ£ņŗ£ļÉśņ¢┤ ņ▓£Ļ│ĄņØś ņ¦äļŗ© ļ░Å ļé┤ņŗ£Ļ▓Į ņ╣śļŻī Ēøä ĒÅēĻ░ĆņŚÉ ļÅäņøĆņØ┤ ļÉ£ļŗż. ļé┤ņŗ£Ļ▓Į ņŗ£ņłĀ Ēøä ņØśņØĖņä▒ ņ▓£Ļ│ĄņØ┤ ņŚåņØ┤ ņ×æņØĆ ĻĖ░ĒżĻ░Ć Ļ┤Ćņ░░ļÉĀ ņłś ņ׳ņ£╝ļ»ĆļĪ£, ņśüņāü Ļ▓Ćņé¼ņŚÉņä£ ĒÖĢņØĖļÉśļŖö ņØ┤ņāüļōżņØĆ ļ░śļō£ņŗ£ ļé┤ņŗ£Ļ▓Į Ļ▓Ćņé¼ ļ░Å ņ×äņāü ņ”ØņāüĻ│╝ ĒĢ©Ļ╗ś ĒÅēĻ░ĆļÉśņ¢┤ņĢ╝ ĒĢ£ļŗż[3,11].
ERCP ņŚ░Ļ┤Ć ņ▓£Ļ│ĄņØĆ ņ▓£Ļ│ĄņØś ņ£äņ╣śņŚÉ ļö░ļØ╝ ĒīĮļīĆļČĆļź╝ ĒżĒĢ©ĒĢ£ ņĘīļŗ┤Ļ┤Ć ņ▓£Ļ│ĄĻ│╝ ņŗŁņØ┤ņ¦ĆņןņØś ļ╣ä ĒīĮļīĆļČĆ ņ▓£Ļ│Ąņ£╝ļĪ£ ļČäļźśļÉśĻ│Ā, ņ╣śļŻī ļ░®ņŗØĻ│╝ ņśłĒøäņŚÉ ņ░©ņØ┤Ļ░Ć ņ׳ļŗż.
ERCPņÖĆ Ļ┤ĆļĀ©ļÉ£ ņ▓£Ļ│ĄņØś ņ£äņ╣śļŖö StapferņØś ļČäļźśļ▓ĢņŚÉ ņØśĻ▒░ĒĢśņŚ¼ ņ£äĒŚśļÅä ņł£ņä£ņŚÉ ļö░ļØ╝ 4Ļ░Ćņ¦ĆļĪ£ ĻĄ¼ļČäĒĢ£ļŗż(Table 1) [12]. 1ĒśĢ ņ▓£Ļ│ĄņØĆ ļé┤ņŗ£Ļ▓Į ņ×Éņ▓┤ņŚÉ ņØśĒĢ£ ņŗŁņØ┤ņ¦ĆņןņØś ņÖĖņĖĪ ļ▓ĮņØś ņåÉņāüņ£╝ļĪ£ ERCP ņŚ░Ļ┤Ć ņ▓£Ļ│ĄņØś 15-20%ļź╝ ņ░©ņ¦ĆĒĢ£ļŗż. 2ĒśĢ ļ░Å 3ĒśĢ ņ▓£Ļ│ĄņØĆ ERCP ņŚ░Ļ┤Ć ņ▓£Ļ│ĄņØś 80-85%ļź╝ ņ░©ņ¦ĆĒĢśļ®░ ņ£ĀļæÉ ĒīĮļīĆļČĆ ņŻ╝ņ£äņŚÉ ņŻ╝ļĪ£ ļ░£ņāØĒĢ£ļŗż. 4ĒśĢ ņ▓£Ļ│ĄņØĆ Ēøä ļ│ĄĻ░Ģ ļé┤ņØś Ļ│ĄĻĖ░ļ¦ī Ļ┤Ćņ░░ļÉśļŖö Ļ▓ĮņÜ░ņØ┤ļŗż. 21Ļ░£ņØś ņĀäĒ¢ź ņŚ░ĻĄ¼(16,855ļ¬ģ)ņŚÉ ļīĆĒĢ£ ņ▓┤Ļ│äņĀüņØĖ ļ¼ĖĒŚīĻ│Āņ░░ņŚÉņä£ 0.60%ņØś ĒÖśņ×É(95% confidence interval [CI] 0.48%-0.72%)ņŚÉņä£ ERCPņÖĆ Ļ┤ĆļĀ©ļÉ£ ņŗŁņØ┤ņ¦Ćņן ļśÉļŖö ņĘīļŗ┤Ļ┤Ć ņ▓£Ļ│ĄņØ┤ ļ│┤Ļ│ĀļÉśņŚłņ£╝ļ®░, ņ▓£Ļ│Ą Ļ┤ĆļĀ© ņé¼ļ¦ØļźĀņØĆ 9.90% (95% CI 3.96%-15.84%)ņśĆļŗż[13]. Ļ░Ćņן ņĄ£ĻĘ╝ ļ░£Ēæ£ļÉ£ ņ▓┤Ļ│äņĀüņØĖ ļ¼ĖĒŚīĻ│Āņ░░ņŚÉņä£ļÅä 0.60%ņØś ļÅÖņØ╝ĒĢ£ ņ▓£Ļ│ĄļźĀņØ┤ ļ│┤Ļ│ĀļÉśņŚłļŗż(12Ļ░£ ĒøäĒ¢ź ņŚ░ĻĄ¼, 42,374ļ¬ģ) [14]. ĒĢ£ ĒøäĒ¢ź ņŚ░ĻĄ¼ņŚÉņä£ Stapfer ļČäļźśņØś 2ĒśĢ-4ĒśĢ ņ▓£Ļ│ĄņŚÉņä£ ļŗżņØīĻ│╝ Ļ░ÖņØĆ ņ£äĒŚś ņÜöņåīĻ░Ć ĒÖĢņØĖļÉśņŚłļŗż[15]: ļé┤ņŗ£Ļ▓Į ņ£ĀļæÉ ņĀłĻ░£ņłĀ(odds ratio [OR] 9.0; 95% CI 3.2-28.1), ļŗ┤Ļ┤Ć Ēśæņ░® ļ░Å ĒÖĢņן(OR 7.2; 95% CI 1.84-28.11), ņ┤Øļŗ┤Ļ┤Ć ĒÖĢņן(OR 4.07; 95% CI 1.63-10.18), ņśżļöö Ļ┤äņĢĮĻĘ╝ ĻĖ░ļŖź ņØ┤ņāü(OR 3.8; 95% CI 1.4-11.0), ņŗ£ņłĀ ņŗ£Ļ░äņØś ņŚ░ņן(OR 1.021; 95% CI 1.006-1.036). ļé┤ņŗ£Ļ▓Į ņ£ĀļæÉ ņĀłņĀ£ņłĀņØ┤ ĒĢäņÜöĒĢ£ ņ£ĀļæÉņāü ļ│æļ│ĆņØś ņĪ┤ņ×¼(OR 18.0; p<0.01)ņÖĆ ņśłļ╣ä ņĀłĻ░£ņłĀņØś ņŗ£Ē¢ē(OR 3.0; p=0.04)ņØĆ ļŗżļźĖ ņŚ░ĻĄ¼ņŚÉņä£ ļÅģļ”ĮņĀüņØĖ ņ£äĒŚśņØĖņ×ÉļĪ£ ĒÖĢņØĖļÉśņŚłļŗż[16].
ERCP ņŚ░Ļ┤Ć ņ▓£Ļ│ĄņØĆ ņ¦äļŗ© ņŗ£ņĀÉ, ļé┤Ļ░Ģ ļé┤ ņØ┤ļ¼╝ņ¦ł, ņ▓£Ļ│ĄņØś ņ£ĀĒśĢ(Ēü¼ĻĖ░, ņ£äņ╣ś) ĒÖśņ×ÉņØś ņĀäļ░śņĀüņØĖ ņāüĒā£ ļ░Å ļ│æņøÉ ļé┤ ņ▓£Ļ│ĄņØś ņ╣śļŻīĻ░Ć Ļ░ĆļŖźĒĢ£ ņĀäļ¼ĖĻ░ĆņØś ņĪ┤ņ×¼, ņé¼ņÜ® Ļ░ĆļŖźĒĢ£ ļ┤ēĒĢ® ņןļ╣äņØś ņ£Āļ¼┤ņŚÉ ļö░ļØ╝ ļ│┤ņĪ┤ ņ╣śļŻī, ļé┤ņŗ£Ļ▓ĮņØä ĒåĄĒĢ£ ļ┤ēĒĢ®, ļŗ┤ņ”Ö ļ░░ņĢĪņłĀ, ņłśņłĀ ļō▒ņØä Ļ│ĀļĀżĒĢ£ļŗż. ļīĆļČĆļČäņØś ERCP ņŚ░Ļ┤Ć ņ▓£Ļ│ĄņØĆ ļ╣ä ņłśņłĀņĀüņØĖ ņ╣śļŻīĻ░Ć ĻČīĻ│ĀļÉśņ¦Ćļ¦ī ņŚ¼ĻĖ░ņŚÉļŖö ņŗĀņżæĒĢ£ ņäĀĒāØņØ┤ ĒĢäņÜöĒĢśņŚ¼, StapferņØś ļČäļźśņŚÉ ļö░ļźĖ ņ╣śļŻī ņĢīĻ│Āļ”¼ņ”śņØ┤ ņĀ£ņĢłļÉśņŚłļŗż(Fig. 1). ļé┤ņŗ£Ļ▓Į Ļ▓Ćņé¼ ņóģļŻī Ēøä ņ▓£Ļ│ĄņØ┤ ĒÖĢņØĖļÉśļŖö Ļ▓ĮņÜ░, 1ĒśĢ ņ▓£Ļ│ĄņØĆ ņłśņłĀ ņ╣śļŻīĻ░Ć ņØ╝ņ░© ņ╣śļŻīņØ┤ļŗż. 2ĒśĢ ļ░Å 3ĒśĢ ņ▓£Ļ│ĄņØś Ļ▓ĮņÜ░ 1ĒśĢ ņ▓£Ļ│ĄņŚÉ ļ╣äĒĢ┤ Ēü¼ĻĖ░Ļ░Ć ņ×æĻ│Ā ļ│ĄĻ░Ģ ļé┤ļĪ£ ĒØśļ¤¼ ļéśĻ░ä ņ▓┤ņĢĪļ¤ēļÅä ņāüļīĆņĀüņ£╝ļĪ£ ņĀüņ¢┤ ĒÖśņ×ÉņØś ņāüĒā£Ļ░Ć ņĢłņĀĢņĀüņØ┤ļ®┤ ļ│┤ņĪ┤ņĀüņØĖ ņ╣śļŻīĻ░Ć ņÜ░ņäĀ ĻČīņןļÉ£ļŗż. ļé┤ņŗ£Ļ▓Į Ļ▓Ćņé¼ ņżæņŚÉ ņ▓£Ļ│ĄņØ┤ ĒÖĢņØĖļÉśļŖö Ļ▓ĮņÜ░ ļé┤ņŗ£Ļ▓Į ņłĀĻĖ░ļź╝ ņØ┤ņÜ®ĒĢ£ ļ┤ēĒĢ® Ēś╣ņØĆ ņŖżĒģÉĒŖĖ ņéĮņ×ģ ļō▒ņØ┤ ĻČīĻ│ĀļÉśļ®░, Ļ░ĆļŖźĒĢśļ®┤ ņ”ēņŗ£ ņŗ£ļÅäĒĢśņŚ¼ ļ│Ąļ¦ēņŚ╝ņØä ņśłļ░®ĒĢśĻ│Ā ņłśņłĀ ĒĢäņÜöņä▒ņØä ņżäņØĖļŗż[12,17,18]. ERCP ņŚ░Ļ┤Ć ņ▓£Ļ│ĄņØ┤ ņŻ╝ļĪ£ ļ░£ņāØĒĢśļŖö ļČĆņ£äņØĖ ņŗŁņØ┤ņ¦ĆņןņØĆ ņåīņן ļŗżļźĖ ļČĆņ£ä(Ļ│Ąņן ļ░Å ĒÜīņן)ņŚÉņä£ ļ░£ņāØĒĢśļŖö ņ▓£Ļ│ĄņŚÉ ļ╣äĒĢśņŚ¼ ļåÆņØĆ ņé¼ļ¦ØļźĀņØä ļ│┤ņØĖļŗż. ņØ┤ļ¤¼ĒĢ£ ņé¼ļ¦ØļźĀņØś ņ░©ņØ┤ļŖö ņŗŁņØ┤ņ¦Ćņן ļé┤ņÜ®ļ¼╝ņØś ļłäņČ£ņŚÉ ļīĆĒĢ£ ņĀäņŗĀ ļ░śņØæ ļ░Å ņÖĖĻ│╝ ņłśņłĀ ļ░®ņŗØņØś ņ░©ņØ┤ ļĢīļ¼Ėņ£╝ļĪ£ ņČöņĀĢļÉ£ļŗż. 15Ļ▒┤ņØś ņŗŁņØ┤ņ¦Ćņן ņ▓£Ļ│Ą ņé¼ļĪĆņŚÉ ļīĆĒĢ£ ĒøäĒ¢ź ļČäņäØņŚÉņä£ ņłśņłĀņØ┤ ņ¦ĆņŚ░ļÉśļ®┤(> 24ņŗ£Ļ░ä) ņé¼ļ¦ØļźĀņØ┤ ĻĖēĻ▓®Ē׳ ņ”ØĻ░ĆĒĢ£ļŗżļŖö ņé¼ņŗżņØ┤ ĒÖĢņØĖļÉśņŚłļŗż[19]. ņĀäņ▓┤ ņé¼ļ¦ØļźĀņØĆ 20%ņśĆņ£╝ļ®░, ļŗżļźĖ ņŚ¼ļ¤¼ ņĮöĒśĖĒŖĖņŚÉņä£ļÅä ņ£Āņé¼ĒĢ£ ņé¼ļ¦ØļźĀņØ┤ ļ│┤Ļ│ĀļÉśņŚłļŗż. ņ▓£Ļ│ĄņŚÉ ļīĆĒĢśņŚ¼ ļé┤ņŗ£Ļ▓Į ņ╣śļŻīļź╝ ņŗ£Ē¢ēĒĢśņśĆņØä Ļ▓ĮņÜ░, ņ×ģņøÉ ĻĖ░Ļ░äņØ┤ ņ¦¦ņĢäņ¦ĆļŖö Ļ▓ĮĒ¢źņØ┤ ĒÖĢņØĖļÉśņŚłļŗż[20-22].
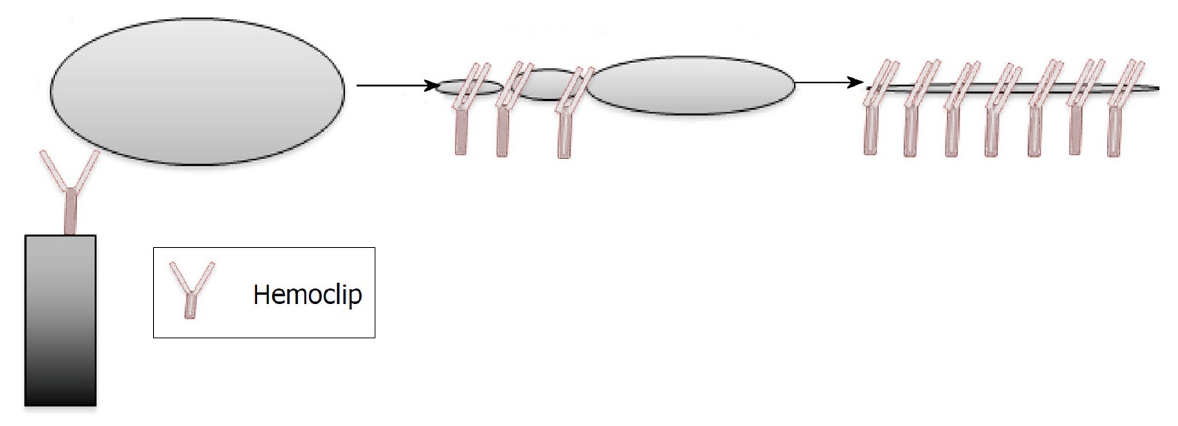
Through-the-scope (TTS) Ēü┤ļ”ĮņØĆ ņ▓£Ļ│ĄņØś Ļ░Ćņןņ×Éļ”¼ļź╝ ļæśļ¤¼ņŗ╝ ņĪ░ņ¦üņØ┤ ļČĆļō£ļ¤ĮĻ│Ā ļ╣äņä¼ņ£Āņä▒ņØĖ Ļ▓ĮņÜ░ ņ£ĀņÜ®ĒĢśļŗż(Fig. 2). ĒĢśņ¦Ćļ¦ī ņØĄĒÅŁņØś ņĀ£ĒĢ£ ļĢīļ¼ĖņŚÉ ņØ╝ļ░śņĀüņ£╝ļĪ£ ņ×æņØĆ Ļ▓░ĒĢ©(< 10 mm)ņŚÉļ¦ī ņĀüņÜ®ĒĢĀ ņłś ņ׳ļŗż[23-25]. ņóĆ ļŹö Ēü░ ņ▓£Ļ│Ą(10-25 mm)ņØĆ over-the-scope (OTS) Ēü┤ļ”Įņ£╝ļĪ£ ņ╣śļŻīĒĢĀ ņłś ņ׳ļŗż(Fig. 3) [23]. 30 mmļ│┤ļŗż Ēü░ ņ▓£Ļ│ĄņØĆ ļé┤ņŗ£Ļ▓Į ņ╣śļŻīĻ░Ć ļŗżņåī ņ¢┤ļĀĄņ¦Ćļ¦ī, OTS Ēü┤ļ”ĮņØ┤ļéś ļé┤ņŗ£Ļ▓Į ļ┤ēĒĢ® ņןļ╣ä(endoscopic suturing device)ļź╝ Ļ┤æļ▓öņ£äĒĢśĻ▓ī ņé¼ņÜ®ĒĢśņŚ¼ ņ╣śļŻīņØś ĒÜ©Ļ│╝ļź╝ ļåÆņØ╝ ņłś ņ׳ļŗż[26-30]. ņĄ£ĻĘ╝ ļ®öĒāĆļČäņäØņŚÉņä£ ņŗŁņØ┤ņ¦Ćņן ņ▓£Ļ│ĄņØś ļé┤ņŗ£Ļ▓Į ņ╣śļŻīņØś ņä▒Ļ│ĄļźĀņØĆ 88%ņŚÉ ņØ┤ļź┤ļŖö Ļ▓āņ£╝ļĪ£ ļ│┤Ļ│Ā ļÉśņŚłļŗż[31]. Artifon ļō▒[32]ņŚÉ ļö░ļź┤ļ®┤ 12ņŗ£Ļ░ä ļé┤ņŚÉ ļé┤ņŗ£Ļ▓Į ņ╣śļŻīļź╝ ņŗ£Ē¢ēĒĢ£ Ļ▓ĮņÜ░ ņ▓£Ļ│ĄņØś ņóģļźś ļ░Å Ēü¼ĻĖ░ņÖĆ ļ¼┤Ļ┤ĆĒĢśĻ▓ī ņ╣śļŻī ņä▒Ļ│ĄļźĀņØĆ 100%ļĪ£ ļ│┤Ļ│ĀļÉśņŚłļŗż. 1, 2ĒśĢ ņ▓£Ļ│ĄņŚÉņä£ 24ņŗ£Ļ░ä ļé┤ņŚÉ ņłśņłĀņĀü ņ╣śļŻīļź╝ ņŗ£Ē¢ēĒĢ£ Ļ▓ĮņÜ░ ņé¼ļ¦ØļźĀņØĆ 6.12%ņśĆņ¦Ćļ¦ī 24ņŗ£Ļ░äņØ┤ Ļ▓ĮĻ│╝ĒĢ£ Ļ▓ĮņÜ░ ņé¼ļ¦ØļźĀņØĆ 17.64%ņŚÉ ļŗ¼ĒĢśņśĆļŗż[14]. ņ▓£Ļ│ĄņŚÉ ļīĆĒĢ£ ļé┤ņŗ£Ļ▓Į ĻĖ░ņłĀņØś ļ░£ņĀä ļ░Å ļŗżņ¢æĒĢ£ Ēü┤ļ”ĮņØś Ļ░£ļ░£ļĪ£ ļé┤ņŗ£Ļ▓Į ņ╣śļŻīņÖĆ ņłśņłĀņĀü ņ╣śļŻīļź╝ Ļ▓░ņĀĢĒĢśļŖö ļŹ░ ļ│æļ│Ć Ēü¼ĻĖ░ņØś ņżæņÜöņä▒ņØĆ ņĀÉņ░© ņżäņ¢┤ļōżĻ│Ā ņ׳ļŗż. ņ▓£Ļ│ĄņØś ļ░£Ļ▓¼ ņŗ£ņĀÉņØ┤ ņ╣śļŻī ļ░®ļ▓ĢņØä Ļ▓░ņĀĢĒĢśļŖö ņżæņÜöĒĢ£ ņÜöņØĖņØ┤ ļÉśņŚłņ£╝ļ®░, ņłśņłĀņĀü ņ▓śņ╣ś ņŚŁņŗ£ ņ╣śļŻī ņŗ£Ļ░äņØ┤ ņ¦ĆņŚ░ļÉśļ®┤ ļČłļ¤ēĒĢ£ ņśłĒøäļź╝ ļ│┤ņØ┤Ļ▓ī ļÉ£ļŗż. ERCP ņŗ£ņłĀ ņżæ Ēś╣ņØĆ ņŗ£ņłĀ Ēøä 12ņŗ£Ļ░ä ļé┤ņŚÉ ļ░£Ļ▓¼ļÉ£ ņ▓£Ļ│ĄņØĆ Ļ░ĆļŖźĒĢ£ ļé┤ņŗ£Ļ▓ĮņĀü ņ╣śļŻīļź╝ ņÜ░ņäĀ ņŗ£ļÅäĒĢ£ļŗż. ļ╣äņ£äĻ┤Ć ļśÉļŖö ļ╣äņŗŁņØ┤ņ¦ĆņןĻ┤Ć ņéĮņ×ģņØĆ Ļ░ÉņĢĢ ļ░Å ņåīĒÖöņĢĪņØś ņĀ£Ļ▒░ņŚÉ ļÅäņøĆņØ┤ ļÉĀ ņłś ņ׳ļŗż. ĻĖ┤ņןņä▒ ĻĖ░ļ│Ąņ”ØņØ┤ ļ░£ņāØĒĢśļ®┤ Ļ░ĆņŖżļĪ£ ņØĖĒĢ£ ĒśłņŚŁĒĢÖ ļČłņĢłņĀĢ Ēś╣ņØĆ ĒśĖĒØĪĻĖ░ ļČĆņĀäņØ┤ ļ░£ņāØĒĢĀ ņłś ņ׳ņ£╝ļ®░ ĻĄ¼ĒÜŹ ņ”ØĒøäĻĄ░ņ£╝ļĪ£ ņ¦äĒ¢ēĒĢĀ ņłś ņ׳ļŗż. Ļ▓ĮĒö╝ņĀüņ£╝ļĪ£ ļīĆĻĄ¼Ļ▓ĮņĀĢļ¦ź ņ╣┤ĒģīĒä░ļź╝ ļ│ĄĻ░Ģ ļé┤ ņéĮņ×ģ Ēøä ļ│ĄļČĆļź╝ ņĢĢļ░ĢĒĢśņŚ¼ ņØæĻĖēņ£╝ļĪ£ Ļ░ÉņĢĢņØä ņłśĒ¢ēĒĢ┤ņĢ╝ ĒĢ£ļŗż[33]. Ļ│ĄĻĖ░ņŚÉ ļ╣äĒĢśņŚ¼ CO2ļŖö ņēĮĻ▓ī ņן ņĀÉļ¦ēņŚÉ ĒØĪņłśļÉśņ¢┤ ĒśĖĒØĪĻĖ░ļź╝ ĒåĄĒĢ┤ ņĀ£Ļ▒░ļÉśļ»ĆļĪ£ ņŗ£ņłĀĻ│╝ Ļ┤ĆļĀ©ļÉ£ ņן ĒīĮņ░Į ļ░Å ļ│ĄĒåĄņØä ņżäņØ╝ ņłś ņ׳ļŗż[34,35]. ņåīĒÖöĻĖ░ ļé┤ņŗ£Ļ▓Į Ļ▓Ćņé¼ņŚÉņä£ CO2ņØś ņé¼ņÜ®ņØĆ Ēæ£ņżĆ Ļ┤ĆĒ¢ēņØ┤ ļÉśņŚłņ£╝ļ®░, ņØśņØĖņä▒ ņ▓£Ļ│ĄņØś ņ£äĒŚśņØ┤ ļåÆņØĆ ņŗ£ņłĀ Ēś╣ņØĆ ņØśņØĖņä▒ ņ▓£Ļ│ĄņØ┤ ņØśņŗ¼ļÉśĻ▒░ļéś ĒÖĢņØĖļÉ£ Ļ▓ĮņÜ░ ļŹöņÜ▒ ņżæņÜöĒĢśļŗż. ņØśņØĖņä▒ ņ▓£Ļ│ĄņØś ļé┤ņŗ£Ļ▓Į ļ┤ēĒĢ® Ēøä ņśłņāüļÉśļŖö ņŗ£ņłĀņØś ņä▒Ļ│ĄļźĀĻ│╝ ĒÖśņ×ÉņØś ņĀäļ░śņĀüņØĖ ņ×äņāü ņāüĒā£ļź╝ Ļ│ĀļĀżĒĢśņŚ¼ ņČöĻ░ĆņĀüņØĖ ņ╣śļŻīĻ░Ć ĻČīņןļÉ£ļŗż. ņØśņØĖņä▒ ņ▓£Ļ│ĄņŚÉ ļīĆĒĢ£ ļé┤ņŗ£Ļ▓Į ņ╣śļŻīĻ░Ć ņŗżĒī©ĒĢśņśĆĻ▒░ļéś ņŗ£ņłĀņØä ņŗ£Ē¢ēĒĢśņ¦Ć ļ¬╗ĒĢśļŖö Ļ▓ĮņÜ░, ĻĘĖļ”¼Ļ│Ā ņ×äņāü ņāüĒā£Ļ░Ć ņĢģĒÖöļÉśļŖö ĒÖśņ×ÉļŖö ņÖĖĻ│╝ ņ╣śļŻīĻ░Ć ĻČīņןļÉ£ļŗż. ņØśņØĖņä▒ ņ▓£Ļ│ĄņØĆ Ļ┤Ćļ”¼Ļ░Ć ļ│Ąņ×ĪĒĢśĻĖ░ ļĢīļ¼ĖņŚÉ ļé┤ņŗ£Ļ▓Į ņĀäļ¼ĖņØś, ņśüņāüņØśĒĢÖĻ│╝ ņĀäļ¼ĖņØś ļ░Å ņÖĖĻ│╝ ņĀäļ¼ĖņØśļź╝ ĒżĒĢ©ĒĢśļŖö ļŗżĒĢÖņĀ£ ņĀæĻĘ╝ņØ┤ ĒĢäņÜöĒĢśļŗż. ņØśņØĖņä▒ ņ▓£Ļ│ĄņØś ĒøäņåŹ ņĪ░ņ╣śļŖö ņ▓£Ļ│ĄņØś ņ£ĀĒśĢĻ│╝ ļČĆņ£ä ļ░Å ĒÖśņ×ÉņØś ņ×äņāü ņāüĒā£ņŚÉ ļö░ļØ╝ ļŗ¼ļØ╝ņ¦äļŗż. ļ│┤ņĪ┤ ņ╣śļŻīļŖö Ļ▓ĮņĀĢļ¦ź ĒĢŁņāØņĀ£, ĻĖłņŗØ, ĒśłņŚŁĒĢÖ ļ¬©ļŗłĒä░ļ¦ü ļ░Å ĻĖ┤ļ░ĆĒĢ£ ļŗżĒĢÖņĀ£ ņČöņĀü Ļ▓Ćņé¼ļĪ£ ĻĄ¼ņä▒ļÉ£ļŗż. ļ╣äĻ▓ĮĻĄ¼ņśüņ¢æņØĆ 7ņØ╝ ņØ┤ņāü ĻĖłņŗØņØ┤ ĒĢäņÜöĒĢśĻ▒░ļéś ņśüņ¢æ Ļ▓░ĒĢŹ ĒÖśņ×ÉņŚÉĻ▓ī ĻČīņןļÉ£ļŗż. ļ│┤ņĪ┤ ņ╣śļŻīĻ░Ć ņŗżĒī©ĒĢśĻ│Ā ĒÖśņ×ÉņØś ņāüĒā£Ļ░Ć ņĢģĒÖöļÉśļ®┤(Ēī©Ēśłņ”Ø ļśÉļŖö ļ│Ąļ¦ēņŚ╝ ņ¦ĢĒøä) ņłśņłĀņØä Ļ░ĢļĀźĒ׳ Ļ│ĀļĀżĒĢ£ļŗż[33,36-38]. ņ▓£Ļ│ĄņØś Ēü¼ĻĖ░Ļ░Ć Ēü¼Ļ▒░ļéś, ļ│Ąļ¦ēņŚ╝ņ£╝ļĪ£ ņØĖĒĢ£ ņĀäņŗĀ ņ”Øņāü, Ēī©Ēśłņ”ØņØś ņ¦äĒ¢ē ļō▒ ņ×äņāü ņāüĒā£ņØś ņĢģĒÖö, ĒÖ£ņä▒ ļłäņČ£ņØś ņĪ┤ņ×¼, Ļ▓ĮĒö╝ ļ░░ņĢĪņØ┤ ņŗżĒī©ĒĢśĻ▒░ļéś Ļ▓ĮĒö╝ ļ░░ņĢĪņØ┤ ļČłĻ░ĆļŖźĒĢ£ ļ¦ÄņØĆ ņ¢æņØś ņןĻ┤Ć ļé┤ņÜ®ļ¼╝ņØ┤ ļ│ĄļČĆ CT Ļ▓Ćņé¼ņŚÉņä£ Ļ┤Ćņ░░ļÉĀ ļĢī ņĪ░ĻĖ░ ņłśņłĀņØ┤ ĻČīņןļÉ£ļŗż. 2, 3ĒśĢņØś ERCP ņŚ░Ļ┤Ć ņ▓£Ļ│ĄņØĆ ļ╣äņłśņłĀņĀü ņ╣śļŻīņŚÉņä£ ļīĆļČĆļČä ĒÜ©Ļ│╝ņĀüņØĖ ļ░śņØæņØä ļ│┤ņØ┤ņ¦Ćļ¦ī, ļ╣äņłśņłĀņĀü ņ╣śļŻīĻ░Ć ņŗżĒī©ĒĢśņŚ¼ ņ¦ĆņŚ░ļÉ£ ņłśņłĀņĀü ņ╣śļŻīļŖö ļČłļ¤ēĒĢ£ ņśłĒøäļź╝ ļ│┤ņØĖļŗż[39,40]. ļ╣äņłśņłĀņĀü ņ╣śļŻī ņŗżĒī©ļĪ£ 24ņŗ£Ļ░äņØ┤ ņ¦ĆņŚ░ļÉśņ¢┤ ņŗ£Ē¢ēļÉ£ ņłśņłĀņĀü ņ▓śņ╣śļŖö ņ▓£Ļ│ĄņØś ņóģļźśņÖĆļŖö ļ¼┤Ļ┤ĆĒĢśĻ▓ī ņØ┤ĒÖśņ£©, ņé¼ļ¦ØļźĀ ļ░Å ņ×¼ņøÉ ĻĖ░Ļ░äņØ┤ ņ”ØĻ░ĆĒĢśļŖö Ļ▓ĮĻ│╝ļź╝ ļ│┤ņØĖļŗż[19,41]. ņØśņØĖņä▒ ņ▓£Ļ│ĄņØś ņÖĖĻ│╝ ņłśņłĀ ļ░®ņŗØ(laparoscopy vs. open procedure)ņØĆ ņŻ╝ļĪ£ ņ▓£Ļ│ĄņØś ņ£äņ╣śņÖĆ ņÖĖĻ│╝ ņØśņé¼ņØś ņäĀĒāØņŚÉ ņØśĒĢ┤ Ļ▓░ņĀĢļÉ£ļŗż.
ņ▓£Ļ│ĄņØ┤ ļ░£ņāØĒĢśļ®┤ ņ×ģņøÉ ļ░Å Ļ┤æļ▓öņ£ä ĒĢŁņāØņĀ£ Ēł¼ņŚ¼ļź╝ ņŗ£Ē¢ēĒĢ£ļŗż. ļ¼ĖĒŚīņŚÉ ļ│┤Ļ│ĀļÉ£ ļīĆļČĆļČäņØś ĒÖśņ×ÉļŖö ņ▓£Ļ│Ą ļČĆņ£äņŚÉ ņ▓┤ņĢĪņØś ļłäņČ£ņØä ņĄ£ņåīĒÖöĒĢśĻĖ░ ņ£äĒĢ┤ ĻĖłņŗØ, ļ╣äņ£äĻ┤Ć(ļśÉļŖö ņŗŁņØ┤ņ¦ĆņןĻ┤Ć) ņéĮņ×ģ, ņ¢æņä▒ņ×ÉĒÄīĒöäņ¢ĄņĀ£ņĀ£ļź╝ Ēł¼ņŚ¼ĒĢśņśĆļŗż. ļé┤ņŗ£Ļ▓ĮņØ┤ļéś ņłśņłĀņØä ĒåĄĒĢ┤ ņ▓£Ļ│ĄņØ┤ ņä▒Ļ│ĄņĀüņ£╝ļĪ£ ļ┤ēĒĢ®ļÉ£ Ļ▓ĮņÜ░ Ļ▓ĮĻĄ¼ ņäŁņĘ©ļź╝ ņŗ£ņ×æĒĢĀ ņłś ņ׳ļŗż. Ļ▓ĮņĀĢļ¦źņśüņ¢æņØĆ ņןĻĖ░Ļ░ä ņןļé┤ ņäŁņĘ©Ļ░Ć ņŚåņØä Ļ▓āņ£╝ļĪ£ ņśłņāüļÉśĻ▒░ļéś ņŗ¼Ļ░üĒĢ£ ņśüņ¢æņŗżņĪ░ņŚÉ Ļ▒Ėļ”░ ĒÖśņ×ÉņŚÉĻ▓ī ĻČīņןļÉ£ļŗż. ņØśņØĖņä▒ ņ▓£Ļ│ĄņØś ņä▒Ļ│ĄņĀüņØĖ ļé┤ņŗ£Ļ▓Į ņ╣śļŻīĻ░Ć ņśłņāüļÉśļ®┤ ļ│Ėļל ļ¬®ņĀüņØ┤ņŚłļŹś ņŗ£ņłĀņØä ņÖäļŻīĒĢśļŖö Ļ▓āņØ┤ ņżæņÜöĒĢĀ ņłś ņ׳ļŗż[42]. ņŗ£ņłĀņØä ņÖäļŻīĒĢśņ¦Ć ņĢŖņØĆ ĒÖśņ×ÉļŖö ņŻ╝ļĪ£ ņĪ░ņĀłļÉśņ¦Ć ņĢŖļŖö ļŗ┤Ļ┤ĆņŚ╝ņ£╝ļĪ£ ņ×äņāü Ļ▓ĮĻ│╝Ļ░Ć ņĢģĒÖöļÉśņ¢┤ ņé¼ļ¦ØĒĢĀ ņłś ņ׳ļŗż[43]. 1ņ░© ļé┤ņŗ£Ļ▓Į ļ┤ēĒĢ®ņØ┤ ņä▒Ļ│ĄĒĢśļ®┤ ņ▓£Ļ│ĄņØś ņ£ĀĒśĢĻ│╝ Ļ┤ĆĻ│äņŚåņØ┤ ņĢĮ 90%ņØś ĒÖśņ×ÉĻ░Ć ņłśņłĀ ņŚåņØ┤ ĒÜīļ│ĄļÉ£ļŗż. ņłśņłĀņØ┤ ĒĢäņÜöĒĢ£ ņØ╝ļ░śņĀüņØĖ ņ¦ĢĒøäņŚÉļŖö ļŗżļ¤ēņØś ņĪ░ņśüņĀ£ ļłäņČ£, ļé┤ņŗ£Ļ▓Įņ£╝ļĪ£ ĒĢ┤Ļ▓░ĒĢĀ ņłś ņŚåļŖö ļ¼ĖņĀ£(ņśł: ņ£ĀļæÉļČĆ ņóģņ¢æņØś ļé┤ņŗ£Ļ▓Į ņ╣śļŻī ņżæ ļ░£ņāØĒĢ£ ņ▓£Ļ│Ą), ņŗ¼ĒĢ£ ļ│Ąļ¦ēņŚ╝, ļ╣äņłśņłĀ ņ╣śļŻīņŚÉļÅä ļČłĻĄ¼ĒĢśĻ│Ā ņŗ¼Ļ░üĒĢ£ Ēī©Ēśłņ”Ø, Ļ▓ĮĒö╝ ļ░░ņĢĪ ļśÉļŖö ļé┤ņŗ£Ļ▓Į ņ┤łņØīĒīī ņ£ĀļÅä ļ░░ņĢĪņØ┤ ļČłĻ░ĆļŖźĒĢ£ Ēøäļ│Ąļ¦ēĻ░Ģļé┤ ņ▓┤ņĢĪ ņĀĆļźś ļō▒ņØ┤ ĒżĒĢ©ļÉ£ļŗż[44,45]. ļ░£ņŚ┤, ļ╣łļ¦ź, ļ│Ąļ▓Į Ļ▓Įņ¦ü, ļ░▒ĒśłĻĄ¼ ņ”ØĻ░Ćņ”ØĻ│╝ Ļ░ÖņØĆ ņ×äņāü ņ¦ĢĒøäļŖö ļ│┤ņĪ┤ ņ╣śļŻīĻ░Ć ņŗżĒī©ĒĢśņśĆņ£╝ļ®░ ņØæĻĖē ņłśņłĀņØ┤ ĒĢäņÜöĒĢ©ņØä ņŗ£ņé¼ĒĢ£ļŗż[33,37,38]. ĒÖśņ×ÉņØś ņ×äņāü ņāüĒā£ļŖö ļ│ĖĻ▓®ņĀüņØĖ ļ│Ąļ¦ēņŚ╝ņØ┤ ļ░£ņāØĒĢ£ Ļ▓ĮņÜ░ņŚÉļ¦ī ņĢģĒÖöļÉĀ ņłś ņ׳ļŗż. ļö░ļØ╝ņä£ ņ×äņāü ņāüĒā£ņŚÉ ņØśņĪ┤ĒĢśļ®┤ ņłśņłĀņØ┤ ņ¦ĆņŚ░ļÉśĻ│Ā, ņØ┤ĒÖśņ£© ļ░Å ņé¼ļ¦ØļźĀņØ┤ ņ”ØĻ░ĆĒĢśĻ▓ī ļÉ£ļŗż[19,46].
ņłśņłĀ ļ░®ņŗØņŚÉļŖö ņ▓£Ļ│ĄņØś ņØ╝ņ░© ļ┤ēĒĢ®ņłĀ, ļ│ĄļČĆ ņäĖņ▓Ö, ļ░░ņĢĪĻ┤Ć Ļ▒░ņ╣ś ļ░Å ņŗŁņØ┤ņ¦Ćņן ņĀäĒÖś ļō▒ņØ┤ Ļ│ĀļĀżļÉ£ļŗż[14]. ņłśņłĀ ļ░®ņŗØ ņé¼ņØ┤ņØś ņĀäĒ¢ź ļ╣äĻĄÉ ņŚ░ĻĄ¼ļŖö ļČłĻ░ĆļŖźĒĢśļ®░ Ļ░Ćņן ņĀüĒĢ®ĒĢ£ ņłśņłĀ ļ░®ņŗØņØĆ ņ▓£Ļ│ĄņØś Ēü¼ĻĖ░ņÖĆ ņ£äņ╣ś, ļ░£ņāØ ņŗ£ņĀÉņŚÉņä£ ņłśņłĀĻ╣īņ¦ĆņØś ņŗ£Ļ░ä, ĒÖśņ×ÉņØś ĻĖ░ņĀĆ ņāüĒā£ ļ░Å Ēśäņ×¼ ņ×äņāü ņāüĒā£ļź╝ Ļ│ĀļĀżĒĢśņŚ¼ Ļ▓░ņĀĢĒĢ£ļŗż.
ņ£ĀļæÉļČĆ ņŻ╝ņ£ä ļ░Å ņĘīļŗ┤Ļ┤Ć ņ▓£Ļ│ĄņØś ĻĄŁņåī ņ╣śļŻīļŖö ņ▓£Ļ│ĄņØś ļ┤ēĒĢ® ļśÉļŖö ņ▓£Ļ│ĄņŚÉņä£ ļŗ┤ņ”ÖņØä ņĀäĒÖśĒĢśņŚ¼ ņ×Éļ░£ņĀüņØĖ ņ╣śņ£Āļź╝ ņ£ĀļÅäĒĢ£ļŗż. 2ĒśĢ ņ▓£Ļ│ĄņØś ņ╣śļŻīļŖö ļŗ┤ņ”Öļ░░ņĢĪņłĀņØä ļŗ©ļÅģņ£╝ļĪ£ ņŗ£Ē¢ēĒĢśĻ▒░ļéś ļé┤ņŗ£Ļ▓Į ļ┤ēĒĢ®ņØä ĒĢ©Ļ╗ś ņŗ£Ē¢ēĒĢ£ļŗż. 2ĒśĢ ļ░Å 3ĒśĢ ņ▓£Ļ│ĄņŚÉņä£ ņ▓£Ļ│Ą ļČĆņ£äļĪ£ļČĆĒä░ ļŗ┤ņ”ÖņØś ņĀäĒÖśņŚÉļŖö ĒöīļØ╝ņŖżĒŗ▒ ņŖżĒģÉĒŖĖ, ņÖäņĀä Ēö╝ļ¦ēĒśĢ ņ×ÉĻ░ĆĒīĮņ░Įņä▒ ĻĖłņåŹņŖżĒģÉĒŖĖ(fully covered self-expandable metal stent, FCSEMS) ļ░Å Ļ▓Įļ╣äļŗ┤ļÅäļ░░ņĢĪļ▓Ģ ļō▒ņØ┤ ņØ┤ņÜ®ļÉ£ļŗż. ņĀĆļźśļÉ£ ņ▓┤ņĢĪņØĆ Ļ▓ĮĒö╝ ļ░░ņĢĪ Ēś╣ņØĆ ļé┤ņŗ£Ļ▓Į ņ┤łņØīĒīī ņ£ĀļÅä ĒĢśņŚÉ ļé┤ļČĆ ļ░░ņĢĪņØä ņŗ£ļÅä ĒĢĀ ņłś ņ׳ļŗż[47].
StapferņØś ļČäļźśļ▓ĢņŚÉ ļö░ļźĖ ņĀ£2ĒśĢ ņŗŁņØ┤ņ¦Ćņן ņ▓£Ļ│ĄņØĆ Ēøäļ│Ąļ¦ēĻ░ĢĻ│╝ ņŚ░Ļ▓░ļÉ£ļŗż. ERCP ņŗ£ņłĀ ņżæņŚÉ 2ĒśĢ ņ▓£Ļ│ĄņØ┤ ĒÖĢņØĖļÉśļ®┤ ņŗ£ņłĀņ×ÉļŖö ņ▓£Ļ│Ą ļČĆņ£äļź╝ ļ¦ēĻ│Ā ļé┤ņŗ£Ļ▓Į ļŗ┤ņ”Ö ļ░░ņĢĪņłĀņØä ņŗ£ļÅäĒĢśņŚ¼ ļŗ┤ņ”Ö ĒØÉļ”äņØä ņ▓£Ļ│Ą ļČĆņ£äņŚÉņä£ ļ®Ćļ”¼ ļ¢©ņ¢┤ļ£©ļĀżņĢ╝ ĒĢ£ļŗż[48]. ņ▓£Ļ│ĄņØś ļ┤ēĒĢ®ņŚÉ ņé¼ņÜ®ļÉśļŖö TTS Ēü┤ļ”ĮņØĆ ņ▓£Ļ│ĄņØś Ēü¼ĻĖ░, ņ£äņ╣ś, ņŗŁņØ┤ņ¦ĆņןĻ▓Į elevatorņŚÉ ņØśĒĢ£ Ēü┤ļ”Į ņĀüņÜ®ņØś ņĀ£ĒĢ£ ļō▒ ĒĢ£Ļ│äĻ░Ć ņĪ┤ņ×¼ĒĢ£ļŗż. ņØ┤ļ¤¼ĒĢ£ ļ¼ĖņĀ£ļź╝ ĒĢ┤Ļ▓░ĒĢśĻĖ░ ņ£äĒĢ┤ ņŚ¼ļ¤¼ Ļ░£ņØś TTS Ēü┤ļ”ĮņØä ņé¼ņÜ®ĒĢśĻ▒░ļéś, ņóĆ ļŹö ņłśņøöĒĢ£ Ēü┤ļ”Į ņĀüņÜ®ņØä ņ£äĒĢśņŚ¼ ņ║Ī ņןņ░® ņ¦üņŗ£Ļ▓Į(cap-fitted endoscope with an axial view)ņØä ņé¼ņÜ®ĒĢ┤ ļ│╝ ņłś ņ׳ļŗż[20] (Fig. 4). ņŗŁņØ┤ņ¦ĆņןĻ▓Į ņĀäņÜ® TTS Ēü┤ļ”Į(duodenoscope-friendly TTS clip)ņØĆ ņŗ£ņłĀņ×ÉņŚÉĻ▓ī ļŹö ļäōņØĆ ņŗ£ņĢ╝ļź╝ ņĀ£Ļ│ĄĒĢśļ®░ elevatorņÖĆ Ļ┤ĆļĀ©ļÉ£ Ēü┤ļ”Į ņĀüņÜ®ņØś ļČłļ”¼ĒĢ©ņØä ĻĘ╣ļ│ĄĒĢśļŖö ļŹ░ ļÅäņøĆņØ┤ ļÉ£ļŗż[49]. Ēü░ ņ▓£Ļ│ĄņØś ļé┤ņŗ£Ļ▓Į ņ╣śļŻīņŚÉļŖö OTS Ēü┤ļ”ĮņØ┤ļéś ļé┤ņŗ£Ļ▓Į ļ┤ēĒĢ® ņןļ╣ä(endoscopic suturing device)ņÖĖņŚÉ ļŗżļźĖ ņ╣śļŻī ļīĆņĢłņ£╝ļĪ£ ļŗ©ņØ╝ ļśÉļŖö ņØ┤ņżæ ņ▒äļäÉ ļé┤ņŗ£Ļ▓ĮņØä ņé¼ņÜ®ĒĢśņŚ¼ TTS Ēü┤ļ”ĮĻ│╝ endoloopļź╝ Ļ░ÖņØ┤ ņĀüņÜ®ĒĢ┤ ļ│╝ ņłś ņ׳ļŗż[50,51] (Fig. 5). Ļ▓Įļ╣ä ļŗ┤ļÅä ļ░░ņĢĪĻ│╝ FCSEMS ņéĮņ×ģņØä ļ╣äĻĄÉĒĢ£ ļæÉ Ļ░£ņØś ļīĆĻĘ£ļ¬© ņŚ░ĻĄ¼ņŚÉņä£ ĒåĄņ”Ø(p=0.005), ņ×¼ņøÉ ĻĖ░Ļ░ä(p=0.053) ļ░Å Ēøäļ│Ąļ¦ēĻ░ĢņØś ļåŹņ¢æ ļ░£ņāØ(p=0.018)ņŚÉņä£ FCSEMS ņéĮņ×ģņłĀņØ┤ ļŹö ļéśņØĆ Ļ▓░Ļ│╝ļź╝ ļ│┤ņŚ¼ņŻ╝ņŚłļŗż(Table 2) [32,48,52-55]. ļŗżļ¤ēņØś ņĪ░ņśüņĀ£ ļłäņČ£ņØ┤ ļ░£ņāØĒĢśņŚ¼ ļ╣äņłśņłĀ ņ╣śļŻī Ēś╣ņØĆ ņ×ÉņŚ░ņĀüņ£╝ļĪ£ ĒĢ┤Ļ▓░ļÉśņ¦Ć ņĢŖļŖö Ļ▓ĮņÜ░ņŚÉļŖö ņØæĻĖēņłśņłĀņØä Ļ│ĀļĀżĒĢ£ļŗż. ņ×äņāüņĀüņ£╝ļĪ£ ņĢłņĀĢļÉ£ ĒÖśņ×ÉņŚÉņä£ 2ĒśĢ ņ▓£Ļ│ĄņØ┤ ņ¦ĆņŚ░ļÉśņ¢┤ ļ░£Ļ▓¼ļÉ£ Ļ▓ĮņÜ░ņŚÉļŖö ļŗżņŗ£ ERCPļź╝ ņŗ£Ē¢ēĒĢśņŚ¼ ļŗ┤ļÅä ņŖżĒģÉĒŖĖļź╝ ņéĮņ×ģĒĢ£ļŗż[56]. ņØ┤ļ¤¼ĒĢ£ ĒÖśņ×ÉņŚÉņä£ ļ░£ņāØĒĢĀ ņłś ņ׳ļŖö ņ¦ĆņåŹļÉśļŖö Ēøäļ│Ąļ¦ēĻ░ĢņØś ņĀĆļźśļÉ£ ņ▓┤ņĢĪņØĆ Ļ▓ĮĒö╝ ļ░░ņĢĪņ£╝ļĪ£ ņ╣śļŻīĒĢĀ ņłś ņ׳ļŗż[8,57]. ļŗ┤ņ”Öņóģ(biloma)ņØ┤ ļ░£ņāØĒĢśņśĆņØä Ļ▓ĮņÜ░ ļé┤ņŗ£Ļ▓Į ņ┤łņØīĒīīļź╝ ņØ┤ņÜ®ĒĢ£ ļé┤ļČĆļ░░ņĢĪ(internal drainage)ņØĆ ĒÜ©Ļ│╝ņĀüņØĖ ņ╣śļŻī ņłśļŗ©ņØ┤ ļÉĀ ņłś ņ׳ļŗż. ņ▓śņØīņŚÉ ļ╣äņłśņłĀ ņ╣śļŻīļź╝ ņŗ£ļÅäĒĢ£ ĒÖśņ×ÉņØś 1%ņŚÉņä£ ņłśņłĀņØ┤ ĒĢäņÜöĒĢśņśĆņ£╝ļ®░, ņØ┤ļ¤¼ĒĢ£ Ļ▓ĮņÜ░ ņé¼ļ¦ØļźĀņØ┤ 38%ļĪ£ ļŹö ļéśņü£ ņśłĒøäļź╝ ļ│┤ņŚ¼ņŻ╝ņŚłļŗż[39]. Stapfer ļČäļźśļ▓ĢņŚÉ ļö░ļźĖ ņĀ£3ĒśĢ ņŗŁņØ┤ņ¦Ćņן ņ▓£Ļ│ĄņØĆ 95%ņØś ĒÖśņ×ÉņŚÉņä£ ņä▒Ļ│ĄņĀüņØĖ ļ╣äņłśņłĀ ņ╣śļŻīĻ░Ć Ļ░ĆļŖźĒĢśļ»ĆļĪ£ ņÜ░ņäĀ ļ│┤ņĪ┤ ņ╣śļŻīļź╝ ņŗ£ļÅäĒĢ£ļŗż. ERCP ņŗ£ņłĀ ņżæņŚÉ ņĘīļŗ┤Ļ┤ĆņŚÉņä£ ņāüļŗ╣ļ¤ēņØś ņĪ░ņśüņĀ£ ņ£ĀņČ£ņØ┤ Ļ░Éņ¦ĆļÉśļ®┤ FCSEMS ļśÉļŖö ĒöīļØ╝ņŖżĒŗ▒ ņŖżĒģÉĒŖĖļź╝ ņé¼ņÜ®ĒĢśņŚ¼ ņ▓£Ļ│ĄļÉ£ ļČĆņ£äņØś Ļ░ÉņĢĢņØä Ļ│ĀļĀżĒĢ£ļŗż[12,58]. ņØ╝ļ░śņĀüņ£╝ļĪ£ 3ĒśĢ ņ▓£Ļ│ĄņØĆ ņóŗņØĆ ņśłĒøäļź╝ ļ│┤ņØĖļŗż[39].
Stapfer ļČäļźśļ▓ĢņŚÉ ļö░ļźĖ ņĀ£1ĒśĢ ņŗŁņØ┤ņ¦Ćņן ņ▓£Ļ│ĄņØĆ ERCP ņŗ£ņłĀ ņżæ ļé┤ņŗ£Ļ▓Į ņŖżņĮźņØś ņĢĢļĀźĻ│╝ ļ¦łņ░░ļĪ£ ņ£Āļ░£ļÉśļ®░ ļ╣äĒīĮļīĆļČĆņ£äņŚÉņä£ ļ░£ņāØĒĢ£ļŗż[12]. ņĄ£ĻĘ╝ ņ▓┤Ļ│äņĀüņØĖ ļ¼ĖĒŚīĻ│Āņ░░ņŚÉ ļö░ļź┤ļ®┤ 1ĒśĢ ņ▓£Ļ│ĄņØĆ ERCP ņŚ░Ļ┤Ć ņ▓£Ļ│Ą ņżæņŚÉņä£ ļæÉ ļ▓łņ¦Ė ļåÆņØĆ ļ╣łļÅäļĪ£ ļ░£ņāØĒĢśņśĆļŗż[14]. Billroth II ņ£äņĀłņĀ£ņłĀņØś Ļ│╝Ļ▒░ļĀźĻ│╝ ĻĖ░ņłĀņĀüņ£╝ļĪ£ ņ¢┤ļĀżņÜ┤ ņŗ£ņłĀņØĆ 1ĒśĢ ņ▓£Ļ│ĄņØś ņŻ╝ņÜö ņ£äĒŚś ņÜöņåīļĪ£ ņĢīļĀżņĀĖ ņ׳ļŗż[16,56,59,60]. ņĄ£ĻĘ╝ ĒøäĒ¢ź ņŚ░ĻĄ¼ņŚÉ ļö░ļź┤ļ®┤ Billroth II ņ£äņĀłņĀ£ņłĀņØä ļ░øņØĆ ĒÖśņ×ÉņŚÉņä£ ļé┤ņŗ£Ļ▓ĮņØś ļŻ©Ēöä ļ¬©ņ¢æ ņéĮņ×ģ(loop-shaped insertion)ņØ┤ ņ▓£Ļ│ĄņØś ņ£äĒŚś ņÜöņåīņ×äņØ┤ ļ░ØĒśĆņĪīļŗż[61].
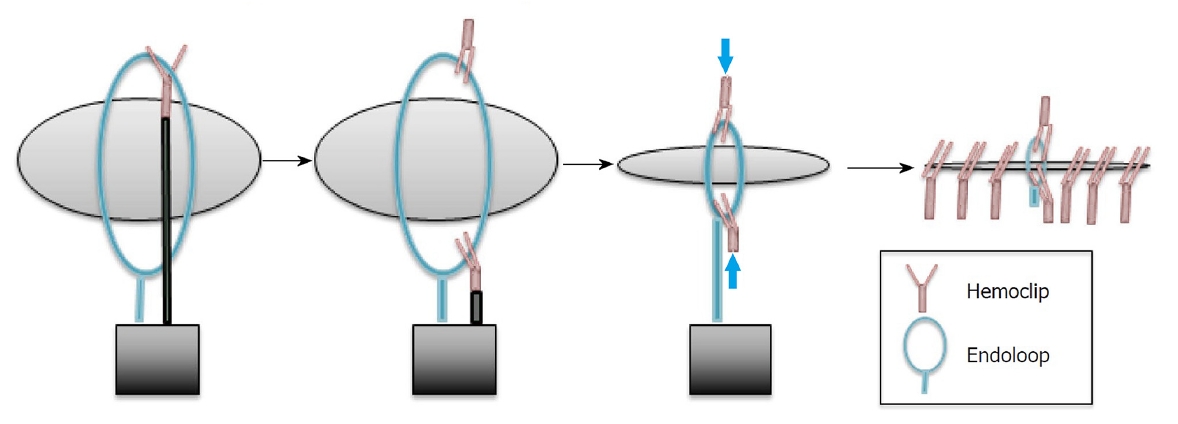
ņØśņØĖņä▒ ņ▓£Ļ│ĄņØ┤ ņŗŁņØ┤ņ¦Ćņן ļ╣äĒīĮļīĆ ļČĆņ£äņŚÉ ņŗ£ņłĀ ņ¦üĒøä ļśÉļŖö ņĪ░ĻĖ░ņŚÉ(< 12 ņŗ£Ļ░ä) ļ░£Ļ▓¼ļÉśļŖö Ļ▓ĮņÜ░ ņÜ░ņäĀ ļé┤ņŗ£Ļ▓Į ņ╣śļŻīĻ░Ć ĻČīņןļÉ£ļŗż. ņĄ£ĻĘ╝ ņä▒Ļ│ĄņĀüņØĖ ļé┤ņŗ£Ļ▓Į ņ╣śļŻī ņé¼ļĪĆĻ░Ć ņ”ØĻ░ĆĒĢśĻ│Ā ņ׳ņ£╝ļ®░ ņØæĻĖē ņłśņłĀņØś ĒĢäņÜöņä▒ņØĆ Ļ░ÉņåīĒĢśĻ│Ā ņ׳ļŗż. ĒĢśņ¦Ćļ¦ī ņ▓£Ļ│ĄņØä ļé┤ņŗ£Ļ▓Įņ£╝ļĪ£ ļ┤ēĒĢ®ĒĢĀ ņłś ņŚåĻ▒░ļéś, ĒÖśņ×ÉĻ░Ć ņāüĒā£Ļ░Ć ņĢģĒÖöļÉśņ¢┤ ļé┤ņŗ£Ļ▓Į ņŗ£ņłĀņØä Ļ▓¼ļö£ ņłś ņŚåļŖö Ļ▓ĮņÜ░ņŚÉļŖö ņØæĻĖē ņłśņłĀņØ┤ ĒĢäņÜöĒĢśļŗż. ļé┤ņŗ£Ļ▓Į ņŗ£ņłĀ Ēøä ņāüļŗ╣ĒĢ£ ņŗ£Ļ░äņØ┤ Ļ▓ĮĻ│╝ĒĢśņŚ¼(> 12ņŗ£Ļ░ä) ņØśņØĖņä▒ ņ▓£Ļ│ĄņØ┤ ņ¦äļŗ©ļÉśĻ│Ā CTņŚÉņä£ ļŗżļ¤ēņØś ņĪ░ņśüņĀ£ ļłäņČ£ņØ┤ ņ׳Ļ▒░ļéś ĒÖśņ×ÉĻ░Ć ļ▓öļ│Ąļ¦ēņŚ╝ ļśÉļŖö Ēī©Ēśłņ”ØņØä ļ│┤ņØ┤ļŖö Ļ▓ĮņÜ░ ņłśņłĀņØ┤ ĒĢäņÜöĒĢśļŗż[14]. ļé┤ņŗ£Ļ▓Į ļ┤ēĒĢ®ņØ┤ ļČłĻ░ĆļŖźĒĢśĻ│Ā ņłśņłĀļÅä ņĀüĒĢ®ĒĢśņ¦Ć ņĢŖņØĆ ĒÖśņ×ÉņŚÉņä£ ļŗżļ¤ēņØś ņĪ░ņśüņĀ£ ļłäņČ£ņØ┤ļéś Ļ│ĀĒśĢļ¼╝ņØ┤ ņŚåļŖö ņĢĪņ▓┤ ņĀĆļźśĻ░Ć ņ׳ņØä ļĢīļŖö Ļ▓ĮĒö╝ ļ░░ņĢĪņØ┤ ĒĢ®ļ”¼ņĀüņØ┤ļŗż[8,62]. ņÖĖĻ│╝ ņ╣śļŻīļŖö ņØ┤ĒÖśņ£©Ļ│╝ ņé¼ļ¦ØļźĀņØ┤ ļåÆņ£╝ļ»ĆļĪ£ ņĀüņØæņ”ØņØ┤ ļÉ£ļŗżļ®┤ Ļ░ĆļŖźĒĢ£ ņ”ēĻ░üņĀüņØĖ ļé┤ņŗ£Ļ▓Į ņ╣śļŻīļź╝ ņÜ░ņäĀņĀüņ£╝ļĪ£ ņäĀĒāØĒĢ£ļŗż. 1ĒśĢ ņ▓£Ļ│ĄņØś ļ┤ēĒĢ®ņŚÉ Ļ░Ćņן ĒØöĒ׳ ņé¼ņÜ®ļÉśļŖö ĻĖ░ĻĄ¼ļŖö Ēü┤ļ”ĮņØ┤ļŗż. ļ╣äĻĄÉņĀü Ēü¼ĻĖ░Ļ░Ć Ēü░ ņ▓£Ļ│ĄņØś Ļ▓ĮņÜ░, TTS Ēü┤ļ”Įļ¦īņ£╝ļĪ£ļÅä ņČ®ļČäĒĢĀ ļĢīļÅä ņ׳ņ¦Ćļ¦ī[21,63], endoloopņÖĆ TTS Ēü┤ļ”ĮņØä ĒĢ©Ļ╗ś ņé¼ņÜ®ĒĢśļ®┤ ņóĆ ļŹö ņä▒Ļ│ĄņĀüņ£╝ļĪ£ ļ┤ēĒĢ®ĒĢĀ ņłś ņ׳ļŗż[22,51] (Fig. 6). ņĄ£ĻĘ╝ņŚÉļŖö OTS Ēü┤ļ”ĮņØä ņĀüņÜ®ĒĢśņŚ¼ ņĄ£ļīĆ ņ¦üĻ▓Į 20 mmņØś ņ▓£Ļ│ĄņØä ļ┤ēĒĢ®ĒĢĀ ņłś ņ׳ņ£╝ļ®░, Ļ▓ĮņÜ░ņŚÉ ļö░ļØ╝ Ēü┤ļ”Į 2Ļ░£ļź╝ ņé¼ņÜ®ĒĢśĻĖ░ļÅä ĒĢ£ļŗż[64,65]. ĒĢ£ ĒøäĒ¢ź ņŚ░ĻĄ¼ņŚÉņä£ OTS Ēü┤ļ”ĮņØä ļÅäņ×ģĒĢ£ Ēøä ņ£äņןĻ┤ĆņØś ņØśņØĖņä▒ ņ▓£Ļ│ĄņØä ņ£äĒĢ£ ņłśņłĀņØ┤ 62.5%ņŚÉņä£ 12.5%ļĪ£ Ļ░ÉņåīĒĢ©ņØä ļ│┤Ļ│ĀĒĢśņśĆļŗż[66]. Covered ļ░Å semi-covered SEMSņØś ņé¼ņÜ®ņØĆ Ēśäņ×¼ ņāüļČĆņ£äņןĻ┤Ć ņ▓£Ļ│ĄņØś ņāłļĪ£ņÜ┤ ņ╣śļŻī ļīĆņĢłņ£╝ļĪ£ ņŚ░ĻĄ¼ļÉśĻ│Ā ņ׳ņ£╝ļ®░, Ē¢źĒøä ņØśņØĖņä▒ ņ▓£Ļ│Ą ņ╣śļŻīņŚÉ Ļ░ĆļŖźĒĢ£ ļÅäĻĄ¼ļĪ£ ĻĖ░ļīĆļÉśĻ│Ā ņ׳ļŗż[67]. 1ĒśĢ ņ▓£Ļ│ĄņØś ņä▒Ļ│ĄņĀüņØĖ ļé┤ņŗ£Ļ▓Į ņ╣śļŻīĻ░Ć ņ”ØĻ░ĆĒĢ©ņŚÉ ļö░ļØ╝ ERCP ņŚ░Ļ┤Ć ņ▓£Ļ│ĄņŚÉņä£ ņ╣śļŻī ņĢīĻ│Āļ”¼ņ”śņØś ņłśņĀĢņØ┤ ņÜöĻĄ¼ļÉśĻ│Ā ņ׳ļŗż[40].
ERCP ņŚ░Ļ┤Ć ņ▓£Ļ│ĄņØĆ ļ░£ņāØ ļ╣łļÅäļŖö ļé«ņ¦Ćļ¦ī ņé¼ļ¦ØļźĀņØ┤ 10%Ļ╣īņ¦Ć ļ│┤Ļ│ĀļÉśļŖö ņ£äņżæĒĢ£ ĒĢ®ļ│æņ”ØņØ┤ļŗż. ļīĆĻĘ£ļ¬©ņØś ņĀäĒ¢ź ņŚ░ĻĄ¼Ļ░Ć ļČłĻ░ĆļŖźĒĢśņŚ¼ ĻĄ¼ņ▓┤ņĀüņØĖ ņ╣śļŻī ļ░®ņ╣©ņØä ņĀ£Ļ│ĄĒĢśļŖö Ļ░ĆņØ┤ļō£ļØ╝ņØĖņØ┤ ņĪ┤ņ×¼ĒĢśņ¦Ć ņĢŖļŖöļŗż. ņĄ£ĻĘ╝ Ļ░£ņĀĢļÉ£ ESGE ĻČīĻ│ĀņĢłņØĆ ļé┤ņŗ£Ļ▓Į ņĀäļ¼ĖņØśĻ░Ć ņØśņØĖņä▒ ņ▓£Ļ│Ą ĒÖśņ×Éļź╝ ņ╣śļŻīĒĢśļŖö ļŹ░ ļÅäņøĆņØä ņżä ņłś ņ׳ļŖö ņĀĢļ│┤ļź╝ ņĀ£Ļ│ĄĒĢśĻĖ░ ņ£äĒĢ£ ļ¬®ņĀüņ£╝ļĪ£ ņ×æņä▒ļÉśņŚłņ£╝ļéś, Ļ░ĆņØ┤ļō£ļØ╝ņØĖņØ┤ ņĢäļŗłĻĖ░ ļĢīļ¼ĖņŚÉ ļ▓ĢņĀüņØĖ ņ╣śļŻī ĻĖ░ņżĆņØä ņäżņĀĢĒĢśļŖö ļŹ░ ņØ┤ņÜ®ĒĢĀ ņłś ņŚåļŗż. ļ│Ė ĻČīĻ│ĀņĢłņØĆ ĻĘ╝Ļ▒░ņŚÉ ĻĖ░ļ░śĒĢ£ ņĄ£ņäĀņØś ĒĢ┤Ļ▓░ ļ░®ņĢłņØä ņĀ£ņŗ£ĒĢśĻ│Ā ņ׳ņ£╝ļéś ļ¬©ļōĀ ņāüĒÖ®ņŚÉ ņØ╝Ļ┤ä ņĀüņÜ®ĒĢĀ ņłśļŖö ņŚåņ£╝ļ®░ ĒŖ╣ņĀĢ ņ×äņāü ņāüĒÖ® ļ░Å ņØ┤ņÜ® Ļ░ĆļŖźĒĢ£ ņןļ╣ä, ņØĖļĀź ļō▒ņØä ņóģĒĢ®ņĀüņ£╝ļĪ£ Ļ│ĀļĀżĒĢ┤ņä£ ĒīÉļŗ©ĒĢ┤ņĢ╝ ĒĢ£ļŗż. ļ│Ė ĻČīĻ│ĀņĢłņØ┤ Ē¢źĒøä ERCP ņŚ░Ļ┤Ć ņ▓£Ļ│ĄņØś ņŗĀņåŹĒĢ£ ņ¦äļŗ©Ļ│╝ ņĀüņĀłĒĢ£ ņ╣śļŻīņŚÉ ļÅäņøĆņØ┤ ļÉśĻĖĖ ĻĖ░ļīĆĒĢ£ļŗż.
REFERENCES
1. Paspatis GA, Arvanitakis M, Dumonceau JM, et al. Diagnosis and management of iatrogenic endoscopic perforations: European Society of Gastrointestinal Endoscopy (ESGE) position statement - update 2020. Endoscopy 2020;52:792ŌĆō810.


2. Cotton PB, Eisen GM, Aabakken L, et al. A lexicon for endoscopic adverse events: report of an ASGE workshop. Gastrointest Endosc 2010;71:446ŌĆō454.


3. Baron TH, Wong Kee Song LM, Zielinski MD, Emura F, Fotoohi M, Kozarek RA. A comprehensive approach to the management of acute endoscopic perforations (with videos). Gastrointest Endosc 2012;76:838ŌĆō859.


4. Jin YJ, Jeong S, Kim JH, et al. Clinical course and proposed treatment strategy for ERCP-related duodenal perforation: a multicenter analysis. Endoscopy 2013;45:806ŌĆō812.


5. Polydorou A, Vezakis A, Fragulidis G, Katsarelias D, Vagianos C, Polymeneas G. A tailored approach to the management of perforations following endoscopic retrograde cholangiopancreatography and sphincterotomy. J Gastrointest Surg 2011;15:2211ŌĆō2217.


6. Sdralis EIK, Petousis S, Rashid F, Lorenzi B, Charalabopoulos A. Epidemiology, diagnosis, and management of esophageal perforations: systematic review. Dis Esophagus 2017;30:1ŌĆō6.

7. Carr-Locke DL. The changing management of colonoscopy-associated perforations. Digestion 2008;78:216ŌĆō217.


8. McCarthy CJ, Butros SR, Dawson SL, Arellano RS. Image-guided percutaneous management of duodenal perforation following endoscopic retrograde cholangiopancreatography (ERCP): assessment of efficacy and safety. Clin Radiol 2018;73:319.e9ŌĆō319.e15.

9. Kim DH, Pickhardt PJ, Taylor AJ, Menias CO. Imaging evaluation of complications at optical colonoscopy. Curr Probl Diagn Radiol 2008;37:165ŌĆō177.


10. Furukawa A, Sakoda M, Yamasaki M, et al. Gastrointestinal tract perforation: CT diagnosis of presence, site, and cause. Abdom Imaging 2005;30:524ŌĆō534.

11. Tamiya Y, Nakahara K, Kominato K, et al. Pneumomediastinum is a frequent but minor complication during esophageal endoscopic submucosal dissection. Endoscopy 2010;42:8ŌĆō14.


12. Stapfer M, Selby RR, Stain SC, et al. Management of duodenal perforation after endoscopic retrograde cholangiopancreatography and sphincterotomy. Ann Surg 2000;232:191ŌĆō198.



13. Andriulli A, Loperfido S, Napolitano G, et al. Incidence rates of post-ERCP complications: a systematic survey of prospective studies. Am J Gastroenterol 2007;102:1781ŌĆō1788.

14. Cirocchi R, Kelly MD, Griffiths EA, et al. A systematic review of the management and outcome of ERCP related duodenal perforations using a standardized classification system. Surgeon 2017;15:379ŌĆō387.


15. Enns R, Eloubeidi MA, Mergener K, et al. ERCP-related perforations: risk factors and management. Endoscopy 2002;34:293ŌĆō298.

16. Weiser R, Pencovich N, Mlynarsky L, et al. Management of endoscopic retrograde cholangiopancreatography-related perforations: experience of a tertiary center. Surgery 2017;161:920ŌĆō929.


17. Raju GS, Fritscher-Ravens A, Rothstein RI, et al. Endoscopic closure of colon perforation compared to surgery in a porcine model: a randomized controlled trial (with videos). Gastrointest Endosc 2008;68:324ŌĆō332.


18. Schmidt A, Fuchs KH, Caca K, K├╝llmer A, Meining A. The endoscopic treatment of iatrogenic gastrointestinal perforation. Dtsch Arztebl Int 2016;113:121ŌĆō128.



19. Avgerinos DV, Llaguna OH, Lo AY, Voli J, Leitman IM. Management of endoscopic retrograde cholangiopancreatography: related duodenal perforations. Surg Endosc 2009;23:833ŌĆō838.


20. Lee TH, Bang BW, Jeong JI, et al. Primary endoscopic approximation suture under cap-assisted endoscopy of an ERCP-induced duodenal perforation. World J Gastroenterol 2010;16:2305ŌĆō2310.

21. Parlak E, K├Čksal A, Di┼¤ibeyaz S, ├£sk├╝dar O, ┼×a┼¤maz N. Endoscopic closure of ERCP-related duodenal perforations by using endoclips: a case series. Surg Laparosc Endosc Percutan Tech 2013;23:e225ŌĆōe228.


22. Ye LP, Mao XL, Zheng HH, et al. Safety of endoscopic resection for duodenal subepithelial lesions with wound closure using clips and an endoloop: an analysis of 68 cases. Surg Endosc 2017;31:1070ŌĆō1077.


23. Stavropoulos SN, Modayil R, Friedel D. Closing perforations and postperforation management in endoscopy: esophagus and stomach. Gastrointest Endosc Clin N Am 2015;25:29ŌĆō45.

24. Daram SR, Tang SJ, Wu R, To SD. Benchtop testing and comparisons among three types of through-the-scope endoscopic clipping devices. Surg Endosc 2013;27:1521ŌĆō1529.


25. L├Īz├Īr G, Paszt A, M├Īn E. Role of endoscopic clipping in the treatment of oesophageal perforations. World J Gastrointest Endosc 2016;8:13ŌĆō22.



26. Haito-Chavez Y, Law JK, Kratt T, et al. International multicenter experience with an over-the-scope clipping device for endoscopic management of GI defects (with video). Gastrointest Endosc 2014;80:610ŌĆō622.


27. Belfiori V, Antonini F, Deminicis S, et al. Successful closure of anastomotic dehiscence after colon-rectal cancer resection using the Apollo overstitch suturing system. Endoscopy 2017;49:823ŌĆō824.


28. Modayil R, Friedel D, Stavropoulos SN. Endoscopic suture repair of a large mucosal perforation during peroral endoscopic myotomy for treatment of achalasia. Gastrointest Endosc 2014;80:1169ŌĆō1170.


29. Iabichino G, Eusebi LH, Palamara MA, et al. Performance of the over-the-scope clip system in the endoscopic closure of iatrogenic gastrointestinal perforations and post-surgical leaks and fistulas. Minerva Gastroenterol Dietol 2018;64:75ŌĆō83.


30. Kobara H, Mori H, Nishiyama N, et al. Over-the-scope clip system: a review of 1517 cases over 9 years. J Gastroenterol Hepatol 2019;34:22ŌĆō30.


31. Verlaan T, Voermans RP, van Berge Henegouwen MI, Bemelman WA, Fockens P. Endoscopic closure of acute perforations of the GI tract: a systematic review of the literature. Gastrointest Endosc 2015;82:618ŌĆō628.e5.


32. Artifon EL, Minata MK, Cunha MA, et al. Surgical or endoscopic management for post-ERCP large transmural duodenal perforations: a randomized prospective trial. Rev Gastroenterol Peru 2015;35:313ŌĆō317.

33. Alfieri S, Rosa F, Cina C, et al. Management of duodeno-pancreato-biliary perforations after ERCP: outcomes from an Italian tertiary referral center. Surg Endosc 2013;27:2005ŌĆō2012.


34. Kim SY, Chung JW, Kim JH, et al. Carbon dioxide insufflation during endoscopic resection of large colorectal polyps can reduce post-procedure abdominal pain: a prospective, double-blind, randomized controlled trial. United European Gastroenterol J 2018;6:1089ŌĆō1098.



35. Baniya R, Upadhaya S, Khan J, et al. Carbon dioxide versus air insufflation in gastric endoscopic submucosal dissection: a systematic review and meta-analysis of randomized controlled trials. Clin Endosc 2017;50:464ŌĆō472.



36. Swan MP, Bourke MJ, Moss A, Williams SJ, Hopper A, Metz A. The target sign: an endoscopic marker for the resection of the muscularis propria and potential perforation during colonic endoscopic mucosal resection. Gastrointest Endosc 2011;73:79ŌĆō85.

37. Knudson K, Raeburn CD, McIntyre RC Jr, et al. Management of duodenal and pancreaticobiliary perforations associated with periampullary endoscopic procedures. Am J Surg 2008;196:975ŌĆō982.


38. Enns R, Branch MS. Management of esophageal perforation after therapeutic upper gastrointestinal endoscopy. Gastrointest Endosc 1998;47:318ŌĆō320.

39. Vezakis A, Fragulidis G, Polydorou A. Endoscopic retrograde cholangiopancreatography-related perforations: diagnosis and management. World J Gastrointest Endosc 2015;7:1135ŌĆō1141.



40. Wu HM, Dixon E, May GR, Sutherland FR. Management of perforation after endoscopic retrograde cholangiopancreatography (ERCP): a population-based review. HPB (Oxford) 2006;8:393ŌĆō399.



41. Patil NS, Solanki N, Mishra PK, Sharma BC, Saluja SS. ERCP-related perforation: an analysis of operative outcomes in a large series over 12 years. Surg Endosc 2020;34:77ŌĆō87.


42. Kayhan B, Akdo─¤an M, Sahin B. ERCP subsequent to retroperitoneal perforation caused by endoscopic sphincterotomy. Gastrointest Endosc 2004;60:833ŌĆō835.


43. Srivastava S, Sharma BC, Puri AS, Sachdeva S, Jain L, Jindal A. Impact of completion of primary biliary procedure on outcome of endoscopic retrograde cholangiopancreatographic related perforation. Endosc Int Open 2017;5:E706ŌĆōE709.



44. Ercan M, Bostanci EB, Dalgic T, et al. Surgical outcome of patients with perforation after endoscopic retrograde cholangiopancreatography. J Laparoendosc Adv Surg Tech A 2012;22:371ŌĆō377.


45. Machado NO. Management of duodenal perforation post-endoscopic retrograde cholangiopancreatography. When and whom to operate and what factors determine the outcome? A review article. JOP 2012;13:18ŌĆō25.

46. Kim BS, Kim IG, Ryu BY, et al. Management of endoscopic retrograde cholangiopancreatography-related perforations. J Korean Surg Soc 2011;81:195ŌĆō204.



47. Arvanitakis M, Dumonceau JM, Albert J, et al. Endoscopic management of acute necrotizing pancreatitis: European Society of Gastrointestinal Endoscopy (ESGE) evidence-based multidisciplinary guidelines. Endoscopy 2018;50:524ŌĆō546.


48. Shi D, Yang JF, Liu YP. Endoscopic treatment of endoscopic retrograde cholangiopancreatography-related duodenal perforations. J Laparoendosc Adv Surg Tech A 2019;29:385ŌĆō391.


49. Aranez JL, Miller J, Hughes M, DeCross A, Kaul V. A novel, duodenoscope-friendly endoscopic clip for treating massive upper-GI bleeding secondary to a Dieulafoy lesion. VideoGIE 2018;3:205ŌĆō206.



50. Samarasena JB, Nakai Y, Park DH, Iwashita T, Chang K. Endoscopic closure of an iatrogenic duodenal perforation: a novel technique using endoclips, endoloop, and fibrin glue. Endoscopy 2012;44(Suppl 2 UCTN):E424ŌĆōE425.


51. Nakagawa Y, Nagai T, Soma W, et al. Endoscopic closure of a large ERCP-related lateral duodenal perforation by using endoloops and endoclips. Gastrointest Endosc 2010;72:216ŌĆō217.


52. Bill JG, Smith Z, Brancheck J, et al. The importance of early recognition in management of ERCP-related perforations. Surg Endosc 2018;32:4841ŌĆō4849.


53. Tringali A, Pizzicannella M, Andrisani G, et al. Temporary FC-SEMS for type II ERCP-related perforations: a case series from two referral centers and review of the literature. Scand J Gastroenterol 2018;53:760ŌĆō767.


54. Trikudanathan G, Hoversten P, Arain MA, Attam R, Freeman ML, Amateau SK. The use of fully-covered self-expanding metallic stents for intraprocedural management of postsphincterotomy perforations: a single-center study (with video). Endosc Int Open 2018;6:E73ŌĆōE77.



55. Odemis B, Oztas E, Kuzu UB, et al. Can a fully covered self-expandable metallic stent be used temporarily for the management of duodenal retroperitoneal perforation during ERCP as a part of conservative therapy? Surg Laparosc Endosc Percutan Tech 2016;26:e9ŌĆōe17.


56. Kim J, Lee SH, Paik WH, et al. Clinical outcomes of patients who experienced perforation associated with endoscopic retrograde cholangiopancreatography. Surg Endosc 2012;26:3293ŌĆō3300.


57. Theopistos V, Theocharis G, Konstantakis C, et al. Non-operative management of type 2 ERCP-related retroperitoneal duodenal perforations: a 9-year experience from a single center. Gastroenterology Res 2018;11:207ŌĆō212.



58. Fatima J, Baron TH, Topazian MD, et al. Pancreaticobiliary and duodenal perforations after periampullary endoscopic procedures: diagnosis and management. Arch Surg 2007;142:448ŌĆō455.


59. Miller R, Zbar A, Klein Y, et al. Perforations following endoscopic retrograde cholangiopancreatography: a single institution experience and surgical recommendations. Am J Surg 2013;206:180ŌĆō186.


60. Cotton PB, Garrow DA, Gallagher J, Romagnuolo J. Risk factors for complications after ERCP: a multivariate analysis of 11,497 procedures over 12 years. Gastrointest Endosc 2009;70:80ŌĆō88.


61. Takano S, Fukasawa M, Shindo H, et al. Risk factors for perforation during endoscopic retrograde cholangiopancreatography in post-reconstruction intestinal tract. World J Clin Cases 2019;7:10ŌĆō18.



62. Krishna RP, Singh RK, Behari A, Kumar A, Saxena R, Kapoor VK. Post-endoscopic retrograde cholangiopancreatography perforation managed by surgery or percutaneous drainage. Surg Today 2011;41:660ŌĆō666.

63. Cordova J, Waxman I, Hart J, Semrad C. Double-balloon endoscopic management of iatrogenic perforation in the small bowel. VideoGIE 2016;1:14ŌĆō15.



64. Furukawa K, Miyahara R, Funasaka K, et al. Endoscopic closure of duodenal perforation with the over-the-scope-clipping system. Intern Med 2016;55:3131ŌĆō3135.



65. Kirtane T, Singhal S. Endoscopic closure of iatrogenic duodenal perforation using dual over-the-scope clips. Gastrointest Endosc 2016;83:467ŌĆō468.


66. Khater S, Rahmi G, Perrod G, et al. Over-the-scope clip (OTSC) reduces surgery rate in the management of iatrogenic gastrointestinal perforations. Endosc Int Open 2017;5:E389ŌĆōE394.



The proposed management algorithm for Stapfer type IŌĆÉIII ERCPŌĆÉrelated duodenal perforations. *Broad-spectrum antibiotics are given to all patients [12].

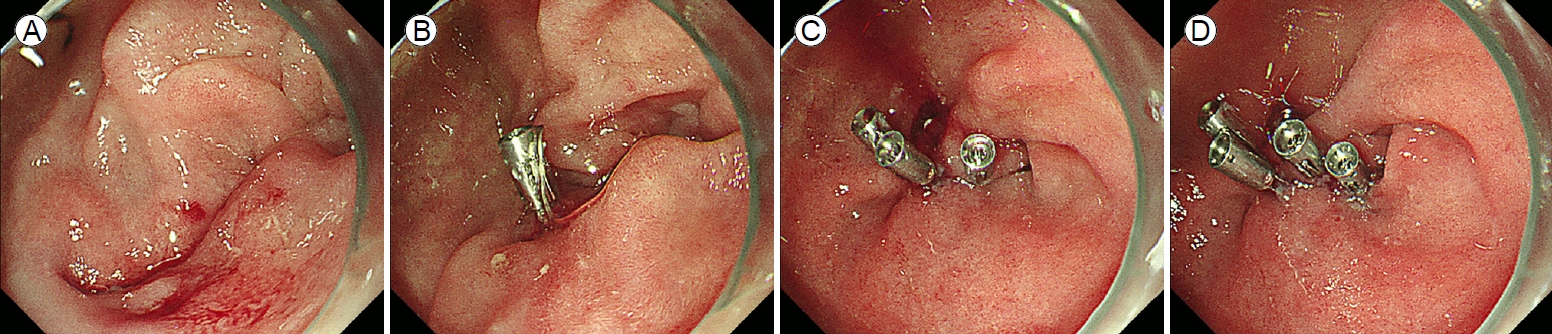
Figure┬Ā1.
(A) A large perforation in the third duodenal region. (B) Application of the first through-the-scope clip. (C) Application of the second and third through-the-scope clips. (D) Successful primary endoscopic closure via cap-assisted endoscopy using multiple endoclips.
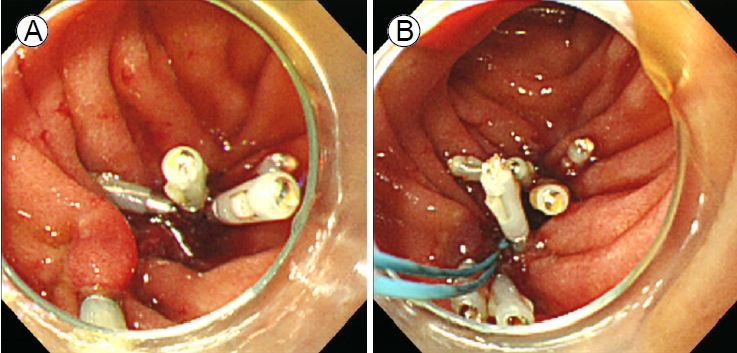
Figure┬Ā4.
(A) Five through-the-scope clips were applied to the
margin of the duodenal perforation. (B) An endoloop was used to approximate the ends of the perforation.
Figure┬Ā6.
Table┬Ā1.
Classification of ERCP-related perforations according to Stapfer et al.
Table┬Ā2.
Previous studies on the endoscopic treatment of Stapfer's type II ERCP-related perforations
| Study | Stapfer | N | Device (n) | Additional percutaneous drainage (n [%]) | Clincal success (n [%]) |
|---|---|---|---|---|---|
| Shi et al. [48] (2019) | II | 44 | NBDC (33) | 13 PD (30%) | 43 (97%) |
| FCSEMS (11) | |||||
| Bill et al. [52] (2018) | II | 17 | PS (9), FCSEMS (8), TTSC (2) | 1 PD (6%) | 16 (94%) |
| Tringali et al. [53] (2018) | II | 16 | FCSEMS (16) | 0 | 16 (100%) |
| Trikudanathan et al. [54] (2018) | II | 15 | FCSEMS (15) | 0 | 15 (100%) |
| Artifon et al. [32] (2015) | II | 12 | TTSCŌĆÉSEMS (12) | 1 PD (8%) | 11 (92%) |
| Odemis et al. [55] (2016) | II | 20 | NBDC (10), FCSEMS plus NBDC (10) | 1 PD (5%) | 19 (95%) |
| Total | 124 | 16 (12.9%) | 120 (96.8%) |




 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print




