INTRODUCTION
The totally implantable port device, or so-called ŌĆ£chemoport,ŌĆØ is placed in the central venous system mainly for parental nutrition, fluid therapy, and infusion of chemotherapeutic agents in patients with oncologic diseases [1,2]. The role of the chemoport in cancer therapy is increasing. This device comprises a radiopaque catheter and an injection port [2]. The subclavian vein, jugular vein, or superior vena cava are accessible central veins for catheter insertion [1]. Several complications associated with such implantations include venous thrombosis, infection, catheter fracture, extravasation, and intravascular dislodgement. The incidence of port catheter dislodgement is low, at 0% to 4.1% [3]. In most patients, the first sign of catheter dislodgement is port dysfunction. It is also detected incidentally when patients undergo periodic routine chest radiographs. The treatment of choice for port dislocation involves immediate retrieval of the distal migrated part, and percutaneous transcatheter retrieval is regarded as the standard method because it is generally easy, safe, and efficient [2,3].
We herein report a case of successful percutaneous transcatheter retrieval of a migrated chemoport in a patient who presented with intermittent palpitation.
CASE REPORT
A 40-year-old female presented with intermittent palpitation. She was referred from the Department of General Surgery after detection of a fractured and dislocated implantable venous port system into the main pulmonary artery.
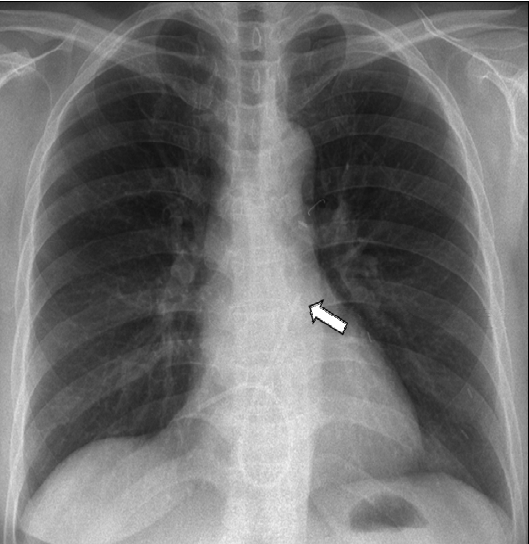
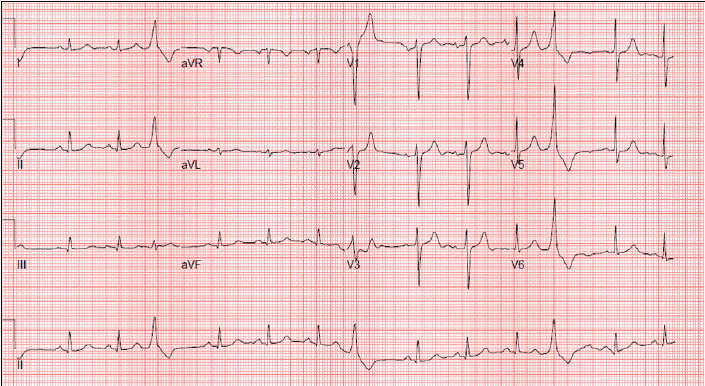
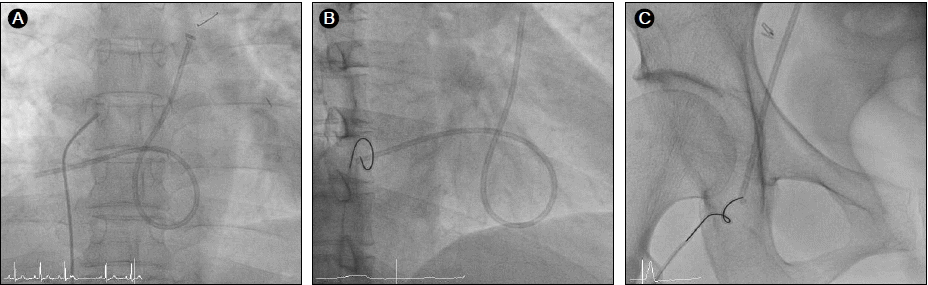
About 17 months previously, she had been diagnosed with a clinical stage IIB (T2N1M0) infiltrating ductal carcinoma in her left breast. During a modified radical mastectomy of the left breast, an 8.5-Fr chemoport (B. Braun Melsungen AG, Melsungen, Germany) was implanted for adjuvant chemotherapy. The implantable central venous device was placed in the right internal jugular vein. After the operation, a chest X-ray revealed good placement of the device. The pathology report revealed an estrogen receptor (ER)-/progesterone receptor (PR)-positive, HER2-overexpressing infiltrating invasive ductal carcinoma without axillary lymph node metastasis. The histological and nuclear grades were III/III and 3/3, respectively. She underwent four cycles of adjuvant chemotherapy with doxorubicin (60 mg/m2) and cyclophosphamide (600 mg/m2) three times weekly. The regimen was then changed to paclitaxel monotherapy. Upon completion of the second cycle of paclitaxel therapy, she complained of chest discomfort. A chest X-ray at that time revealed no significant abnormal findings or catheter position. Because of concurrent elevation of cardiac markers (CK, CK-MB, and TnT), transthoracic echocardiography was performed. Her left ventricular systolic function was mildly decreased with an ejection fraction of 53%, and her left ventricular apex septum was moderately hypokinetic. Coronary angiography was thus performed. Normal coronary arteries were found, confirming stress-induced cardiomyopathy; the patient recovered after 1 month of medical therapy with candesartan 8 mg. There was no evidence of chemoport migration at the time of initial coronary angiography. She continued and completed all scheduled chemotherapy for 18 months. When she visited the outpatient clinic for planned removal of the chemoport after completion of the 18th trastuzumab treatment, she complained of intermittent palpitation. Only the proximal injection port of the chemoport could be removed; the distal catheter part was not evident. A chest radiograph was performed due to suspicion of catheter migration secondary to fracture and compared with the chest CT taken 5 months previously. It showed that the chemoport catheter had migrated from its original location up to the main pulmonary artery, traveling across the right atrium and right ventricle (Fig. 1). An ECG showed premature ventricular complexes, which may have caused the intermittent palpitation due to contact between the catheter and right ventricle (Fig. 2). The patient was immediately sent to the cardiac catheterization room for removal of the migrated fractured catheter. She was placed in the supine position, and retrieval of the dislodged catheter was performed under fluoroscopic guidance. The right common femoral vein was punctured, and an 8-Fr vascular sheath was inserted under local anesthesia with 2% lidocaine. We first attempted to use a 5-Fr multipurpose catheter (ANA M.D., Kyeonggi-do, Korea) to capture the chemoport catheter, but it could not reach to the tip of the fractured catheter (Fig. 3A). Therefore, a 5-Fr pigtail catheter (ANA M.D., Kyeonggi-do, Korea) was advanced to the right atrium, and the fractured chemoport catheter was captured. The pigtail catheter relocated the dislodged fragment to a more favorable position, and a loop snare catheter (St. Jude Medical, Inc., MN, USA) was advanced and captured the proximal tip of the fractured catheter (Fig. 3B). The migrated catheter was grasped and pulled via the inferior vena cava and femoral vein. The chemoport catheter was pulled down into the venous sheath and completely removed with the venous sheath (Fig. 3C). The venous puncture site was manually compressed, and then compression with a sand bag was continued for 2 h. The length of the migrated piece was 22.29 cm, and thrombus formation was not observed at the tip. A plain chest X-ray taken after the retrieval confirmed no residual fragment, and chest CT revealed no evidence of pulmonary thromboembolism. The patient is undergoing careful follow-up and has shown no complications or evidence of tumor recurrence.
DISCUSSION
Various complications of implantable port devices have been reported: pneumothorax, malposition, arrhythmia, skin or systemic infection, extravasation of fluids, occlusion or thrombosis, catheter fracture, and others [2]. Migration is a rare but possible complication of implantable port catheters that requires immediate diagnosis and treatment. The prevalence of catheter migration is 0.4-4% [2]. Since the first report of a migrated catheter fragment by Turner et al. in 1954 [4], port catheter dislodgement has been reported occasionally [1-3,5]. However, the mechanism of catheter migration is not clear. Suggested causes include improper connection between the catheter and port, distortion or angulation of the anastomosis site, use of incorrect equipment, malposition and fatigue of the catheter, and pinch-off syndrome secondary to compression between the clavicle and the first rib [2,3]. The catheter and port are located in the intravascular and extravascular space, respectively, and pressures that compress either the extra- or intravascular component can shift the position of the device. High intrathoracic pressure induced by coughing and straining could cause migration of the port [6]. Rasuli et al. [7] reported a case of catheter migration after excessive flushing. Fracture and/or dislocation of a chemoport catheter have a variety of clinical manifestations. The most common sign is catheter dysfunction, which is detected by increased resistance to infusion. Other symptoms include palpitations, dyspnea, cough, and chest discomfort [2]. Of the 92 cases observed by Cheng et al. [2], 36% were asymptomatic and found incidentally by routine plain chest X-ray. Therefore, patients must be checked regularly by taking chest X-rays at least every 6 months after catheter implantation regardless of symptoms.
The location of the catheter fragments within the cardiovascular system depends on the route of entry, gravity, the stiffness and length of the materials, the flow pattern of the vessel or cardiac chamber, and the position of the patient at the time of the accident [2]. The most commonly reported location of catheter dislodgement is the pulmonary artery, and the most common embolization sites are the right atrium to inferior vena cava and superior vena cava to right atrium [2]. In the present case, the catheter fragment was located in the right atrium and ventricle to the pulmonary artery. Mortality and morbidity differ depending on the location of the catheter fragments. Mortality and morbidity are highest when the fragments are in the right heart, followed by the vena cava; mortality and morbidity are lowest in the pulmonary artery. Causes of death include endocarditis, sepsis, arrhythmia with heart failure, pulmonary thromboembolism, and cardiac wall necrosis [1].
Embolization of the distal fragment in the right cardiac cavity and in the pulmonary artery can produce complications such as arrhythmia, cardiac arrest, and thromboembolism [1]. Therefore, once foreign body embolization has occurred, it must be promptly removed to avoid fatal complications, even if the patient is asymptomatic. Since percutaneous retrieval of a broken guide wire was first introduced by Thomas et al. [8] in 1964, percutaneous endovascular retrieval has become a standard technique for foreign body removal. It is a preferred method with a high success rate of 71% to 100% [9]. Such a high success rate can be achieved by only specialized interventionists.
Many types of equipment have been used to retrieve intravascular foreign bodies, including snares, baskets, grasping forceps, tip-deflecting wires, and balloon catheters. As reported in the literature, the loop snare is the most popular device despite its main disadvantage of poor torque control. When no free end is accessible, a pigtail catheter can be used to reposition the dislodged fragment to the optimal site [2,10]. Chuang et al. [3] reported that the concurrent use of pigtail and loop snare catheters is a feasible and easy method for percutaneous retrieval of a dislodged catheter. Mortality following catheter embolization was 28-57% between 1950 and 1980. However, according to recent studies, the mortality rate has been markedly reduced to 0-1.8% due to the higher success rate of percutaneous retrieval and the advent of more flexible and resilient catheter material [2].
In this case, the patient presented with intermittent palpitation, and chest X-ray confirmed that the chemoport catheter had been dislodged. After carefully questioning her regarding her history, we found that she had received a meridian massage at the insertion site. Therefore, the catheter migration might be ascribable to external compression at the connective site between the port and catheter during the massage. With increases in cancer prevalence, more patients are receiving chemotherapy via chemoports, and more complications, such as catheter dislodgement, are thus expected. Thus, chest X-rays and careful clinical examinations should be performed regularly for early detection and treatment of these complications. Furthermore, patient education for secure management of chemoports is important, as in this case.
In conclusion, initial precise positioning of an implantable port device and a firm connection between the port and the catheter are important to prevent any subsequent disconnection or embolization of the catheter, and frequent performance of chest X-rays is necessary for early detection, even if the patient is asymptomatic. If dislodgement is diagnosed, the device must be removed promptly to avoid fatal complications.



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print






