 |
 |
| Korean J Med > Volume 85(2); 2013 > Article |
|
Abstract
We herein report a case of large cell neuroendocrine carcinoma (NEC) of the gallbladder confirmed by laparoscopic surgery. A 60-year-old male was HBsAg-positive. Abdominal computed tomography showed a 2.5 ├Ś 2.5 cm enhancing polypoid mass in the gallbladder and multiple masses in liver segments 4 and 5 that enhanced in the arterial phase and washed out in the delayed phase. Liver biopsy findings showed only poorly differentiated morphology. A laparoscopic operation was performed for diagnosis of the masses because curative resection seemed impossible to perform, which showed unusual findings of either hepatocelluar carcinoma or gallbladder cancer. Therefore, laparoscopic liver biopsy and cholecystectomy were performed. The final pathologic results of the masses showed large cell NEC of the gallbladder with liver metastasis. Central bisegmentectomy and extensive lymph node dissection were ultimately performed. The patient was still alive 16 months after diagnosis. (Korean J Med 2013;85:183-187)
Primary neuroendocrine carcinoma (NEC) of the gallbladder is very rare. The diagnosis of gallbladder NEC is rarely made preoperatively because this tumor generally presents with nonspecific symptoms [1]. Furthermore, preoperative differentiation between gallbladder adenocarcinoma and gallbladder NEC is not possible with imaging techniques [2].
We herein report a case of large-cell NEC of the gallbladder that manifested as epigastric soreness. It was ultimately diagnosed with laparoscopic surgery in spite of an initial negative ultrasoundguided needle biopsy.
A 60-year-old male presented with epigastric soreness. He had a normal appetite and no history of diarrhea, flushes, or dyspnea. He had no pertinent past medical or surgical history. On physical examination, he was well nourished with stable vital signs and no pallor, jaundice, or significant lymphadenopathy. Abdominal examinations revealed no tenderness, organomegaly, or abnormal masses.
Blood tests revealed an albumin of 3.8 g/dL, AST of 11 U/L, ALT of 10 U/L, alkaline phosphatase of 57 U/L, total bilirubin of 0.6 mg/dL, and prothrombin time of 11.8s (92.5%, 1.04 INR). The viral hepatitis marker status was HbsAg-positive, HbsAb-negative, HbeAg-negative, HbeAb-positive, and anti-HCV-negative. The tumor marker levels were as follows: CEA, 1.8 ng/mL; CA19-9, < 5 U/mL; AFP, 4 IU/mL; and PIVKA-II, 29 mAU/mL.
The chest X-ray findings were within normal limits. Abdominal computed tomography (CT) showed a 2.5 ├Ś 2.5 cm enhancing polypoid mass with a relatively nonenhancing central portion in the fundus of the gallbladder (Fig. 1A). The mass was accompanied by conglomerated, heterogeneously enhancing lymph node enlargement in the hepatoduodenal ligament (Fig. 1B). Also present were multiple low-attenuated masses with arterial enhancement and wash-out and peripheral enhancement on the portal phase in the gallbladder bed (i.e., segments S4 and S5 of the liver) (Fig. 1C and 1D). Positron emission tomography (PET) showed a 2.5-cm hypermetabolic lesion in the gallbladder (pSUV 5.2) and multiple hypermetabolic lesions in the gallbladder bed and hepatoduodenal ligament (pSUV 2.2-7.6). Based on the fact that this patient was an HbsAg-positive carrier and had such unusual CT findings, our presumptive differential diagnosis prior to liver biopsy were gallbladder cancer with liver metastasis or double primary cancer, including hepatocelluar carcinoma and gallbladder cancer.
Ultrasound-guided needle biopsy of the hepatic mass was undertaken in segment 4 of the liver. The results showed no conclusive features with the exception of a very poorly differentiated morphology because of an insufficient specimen. For the purpose of accurate diagnosis of the two masses and curative resection if possible, a laparoscopic operation was performed.
The laparoscopic findings did not show typical findings of either hepatocellular carcinoma or gallbladder cancer; moreover, it seemed impossible to perform curative resection of both masses, including extended cholecystectomy with trisegmentectomy. The cause of inoperability of the masses was the relatively small volume of liver expected to remain after curative resection. Therefore, liver biopsy and cholecystectomy were performed to obtain accurate diagnosis.
On gross examination of the gallbladder, a polypoid, irregularly surfaced, whitish-gray, rubbery to firm mass was found in the fundus of the gallbladder, measuring 2.5 ├Ś 2.5 ├Ś 2.3 cm. There was necrosis in one-third of the cut surface of the mass, with a partly hemorrhagic portion. On microscopic examination, the tumor showed an organoid growth pattern, with solid nests comprising relatively large cells characterized by vesicular nuclei and prominent nucleoli and a variable amount of cytoplasm (Fig. 2A).
Immunohistochemical staining for chromogranin A, synaptophysin, and CD56 disclosed intense and diffusely positive staining in the tumor cells (Fig. 2B-2D). Central bisegmentectomy (S4 and S5) and lymph node dissection were performed 7 days later, and adjuvant chemotherapy with the combination of etoposide and cisplatin was started 30 days later. However, serial follow-up CT scans showed cancer recurrence at the aortocaval and portocaval lymph nodes 9 months after diagnosis. To treat this lymph node recurrence, additional adjuvant chemotherapy with a combination of irinotecan and cisplatin was administered. The patient was still alive 16 months after the diagnosis despite the cancer recurrence in the lymph nodes.
The incidence of NET of the gallbladder has been reported to be approximately 2% to 3% of all gallbladder tumors [1,3]. Both smalland large-cell NEC are poorly differentiated, high-grade NETs with aggressive behavior, and both have a high tendency for early lymph node and distant metastases [4]. The diagnosis of gallbladder NET is rarely made preoperatively because the symptoms at presentation are generally nonspecific, including upper abdominal pain, abdominal discomfort, jaundice, and weight loss. The majority of lesions are incidentally identified at the time of cholecystectomy for cholelithiasis [5]. In our case, similar to those in previous studies [2,6], the patient had no specific symptoms, with the exception of epigastric soreness.
CT reveals no significant differences between NETs and other gallbladder tumors. Although the main findings of high-grade NET of the gallbladder are aggressiveness and/or extensive lymph node involvement, an accurate diagnosis of high-grade NET is potentially problematic because gallbladder adenocarcinoma may present as a huge liver mass with extensive lymph node metastasis at its late stage. A similar presentation is also common for other neoplasms, including cholangiocarcinoma, hepatocelluar carcinoma, or hepatic metastasis involving the gallbladder [1]. However, if a gallbladder tumor presents along with a huge hepatic mass and/or extensive lymphadenopathy at the time of the initial diagnosis, the possibility of high-grade neuroendocrine tumor should be considered [2]. In our case, the gallbladder mass was associated with multiple liver metastases and conglomerated lymphadenopathy along the hepatoduodenal ligament on abdominal CT. Although ultrasound-guided liver biopsy was performed, it showed no additional specific findings with the exception of a poorly differentiated morphology. To accurately diagnose NECs of the gallbladder, more specific staining was required (i.e., immunohistochemistry). The diagnosis of NEC should be confirmed by positive immunohistochemical staining for at least one neuroendocrine marker, such as chromogranin, synaptophysin, or neuron-specific enolase [7]. In the present case, the results of liver biopsy were inconclusive, showing only very poorly differentiated morphology on hematoxylin and eosin staining. Conclusively, laparoscopic cholecystectomy was performed to achieve an accurate diagnosis. It revealed large-cell NEC through positive findings for all markers on immunohistochemical staining, including CD56, chromogranin, and synaptophysin.
Although the prognosis of NEC of the gallbladder is very poor, aggressive surgical resection in combination with chemotherapy could improve the survival outcome if the tumor is resectable [8].
In conclusion, it is difficult to preoperatively differentiate between large cell NEC of the gallbladder and gallbladder adenocarcinoma in spite of various radiological images and needle aspiration biopsy findings. The possibility of NEC of the gallbladder should be considered in cases involving a gallbladder mass with multiple hepatic masses, extensive lymphadenopathy, and poorly differentiated morphology on biopsy, although gallbladder adenocarcinoma could be the main cause of the tumor in this situation. A more active diagnostic work-up for NEC may be required, including immunohistochemistry and, if necessary, laparoscopic surgery.
REFERENCES
1. Eltawil KM, Gustafsson BI, Kidd M, Modlin IM. Neuroendocrine tumors of the gallbladder: an evaluation and reassessment of management strategy. J Clin Gastroenterol 2010;44:687ŌĆō695.


2. Jun SR, Lee JM, Han JK, Choi BI. High-grade neuroendocrine carcinomas of the gallbladder and bile duct: report of four cases with pathological correlation. J Comput Assist Tomogr 2006;30:604ŌĆō609.


3. Duffy A, Capanu M, Abou-Alfa GK, et al. Gallbladder cancer (GBC): 10-year experience at Memorial Sloan-Kettering Cancer Centre (MSKCC). J Surg Oncol 2008;98:485ŌĆō489.


4. Nassar H, Albores-Saavedra J, Klimstra DS. High-grade neuroendocrine carcinoma of the ampulla of vater: a clinicopathologic and immunohistochemical analysis of 14 cases. Am J Surg Pathol 2005;29:588ŌĆō594.


5. Kanakala V, Kasaraneni R, Smith DA, Goulbourne IA. Primary neuroendocrine neoplasm of gallbladder. BMJ Case Rep 2009 May 25 [Epub]. http://dx.doi.org/10.1136/bcr.12.2008.1352



6. Lee JM, Hwang S, Lee SG, et al. Neuroendocrine tumors of the gallbladder: twelve cases in a single institution. Hepatogastroenterology 2010;57:1064ŌĆō1068.

7. Park SY, Lee SH, Kim JY, et al. A case of large cell neuroendocrine carcinoma in the hilar bile duct. Korean J Med 2011;80(Suppl 2):S137ŌĆō141.
Abdominal CT findings. (A) 2.5 ├Ś 2.5 cm enhancing polypoid mass with a relatively nonenhancing central portion in the fundus of the gallbladder was accompanied by irregular thickening of the adjacent gallbladder wall (white arrow). (B) Heterogeneouslyenhancing lymphadenopathy along the hepatoduodenal ligament (black arrow). (C) Multiple arterial enhancement masses in liver segments 4 and 5 (white arrowhead). (D) Multiple masses with wash-out and peripheral enhancement on the portal phase in liver segments 4 and 5 (black arrowheads).
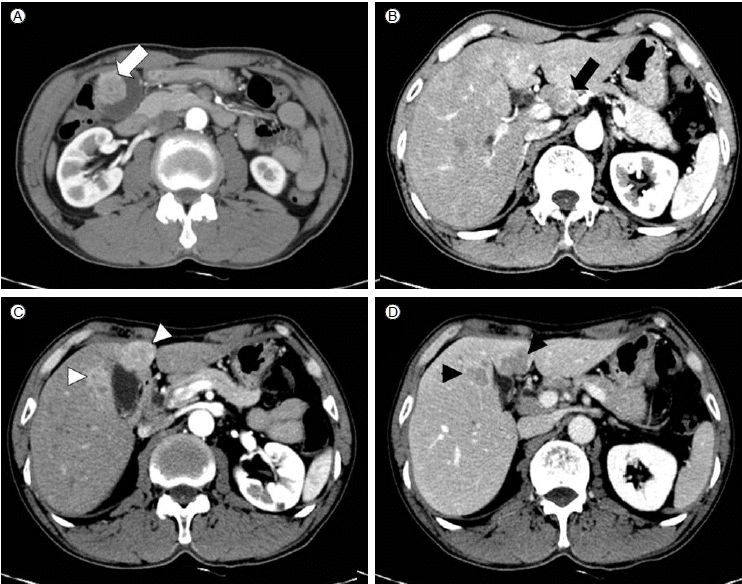
Figure┬Ā1.
Pathologic findings. (A) The tumor shows an organoid growth pattern, with solid nests comprising relatively large cells characterized by vesicular nuclei and prominent nucleoli and a variable amount of cytoplasm (H&E, 400) (left upper corner). (B-D) The tumor cells reveal immunopositivity for CD56 (right upper corner), chromogranin A (left lower corner), and synaptophysin (right lower corner).
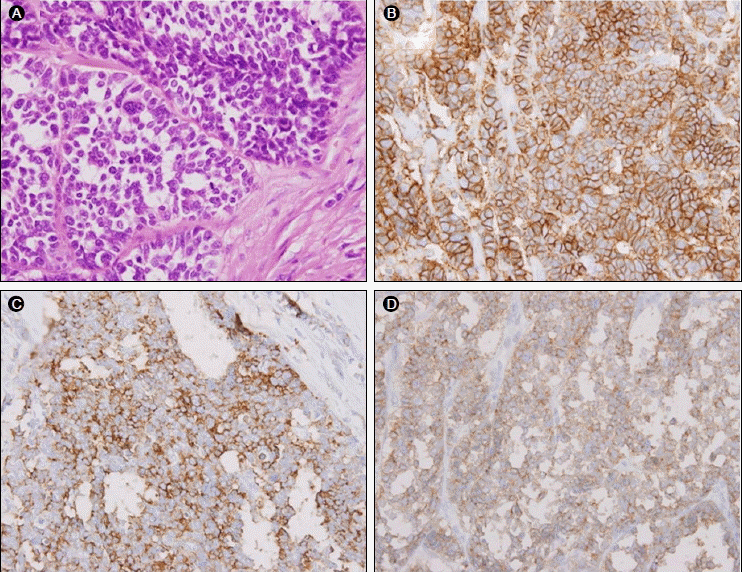
Figure┬Ā2.
-
METRICS

-
- 1 Crossref
- 0 Scopus
- 8,141 View
- 93 Download



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print



