 |
 |
| Korean J Med > Volume 85(3); 2013 > Article |
|
Abstract
Solitary splenic metastases from head and neck cancer are rare. We report a 35-year-old male with nasal cavity cancer with metastasis to the cervical lymph nodes. The patient underwent three cycles of induction chemotherapy, followed by left medial maxillectomy with modified radical neck dissection and concurrent chemoradiotherapy with weekly cisplatin. After 7 months of a disease-free interval, positron-emission tomography showed a high uptake in the spleen, and a biopsy confirmed metastatic carcinoma. After four cycles of systemic chemotherapy with docetaxel and cisplatin, laparoscopic splenectomy was performed. This case highlights that solitary splenic metastasis, although rare, may occur with a locoregionally controlled head and neck cancer and could be treated with local and systemic treatment. (Korean J Med 2013;85:324-328)
Although the prevalence of splenic metastases seems to increase with the improvement of medical imaging techniques, it remains rare [1,2]. Additionally, a solitary splenic lesion as a single site of metastasis from treated solid tumors is a rare occurrence [3]. In head and neck cancer, the lung, bone, and liver were the most common sites of distant metastases [4]. Distant metastasis in head and neck cancer has remained the major cause of mortality and treatment failure, despite better loco-regional control of the disease. Hence, evaluating systemic metastasis is critical. We report a rare case of head and neck cancer metastasizing to the spleen.
A 35-year-old male, who was a non-smoker and a social drinker, was presented to our center with a palpable neck mass. Computed tomography (CT) showed multiple enlarged cervical lymph nodes and a left inferior nasal meatus mass. A nasal cavity biopsy showed malignant cells with the presence of Epstein-Barr virus (EBV) in the tumor cells, favoring undifferentiated carcinoma. In situ hybridization (ISH) demonstrated EBV-encoded small RNA positivity in numerous atypical cells. A whole-body positronemission tomography (PET)/CT scan revealed increased uptake in the left nasal cavity, left level IB, II (Fig. 1). The patient had received three cycles of induction chemotherapy with cisplatin 40 mg/m2 on days 1 and 2, and 5-fluorouracil 1,200 mg/m2 as on days 1 to 4 per 3 weeks. CT evaluation after the second cycle of chemotherapy revealed decreased size of multiple enlarged neck nodes, and a partial response was achieved.
The patient had undergone left medial maxillectomy with left modified radical neck dissection. His pathologic examination was consistent with nasopharyngeal non-keratinizing carcinoma with EBV, and the tumor size was 1.9 ├Ś 0.9 ├Ś 0.7 cm. The resection margin was negative, and 11 metastatic lymph nodes among the 48 lymph nodes were found. Adjuvant chemoradiotherapy was administered with weekly cisplatin 35 mg/m2, with a total of 63 Gy to the left nasal cavity and left level IB, II/IV lymph node region and 56 Gy to the left maxillary sinus, both nasal cavities and left level III, IV/V lymph node region for 6 weeks.
The patient was followed up 1 month after the completion of chemoradiotherapy, and then every 3 months thereafter. After 7 months of disease-free survival, whole-body PET-CT showed increased uptake in the spleen, and abdominal CT demonstrated a 2.5-cm slowly enhancing mass in the spleen without any notable findings in other organs, including the primary site (Fig. 2). There was no splenomegaly or palpable mass in the abdomen, and the patient had no symptoms. Spleen needle biopsy was performed, the splenic nodule was consistent with metastatic carcinoma, and tumor cells were also positive for EBV-ISH (Fig. 3). He received four cycles of systemic chemotherapy with docetaxel and cisplatin. Follow-up abdominal CT revealed a decrease in size of the splenic metastasis; however, the response was stable disease.
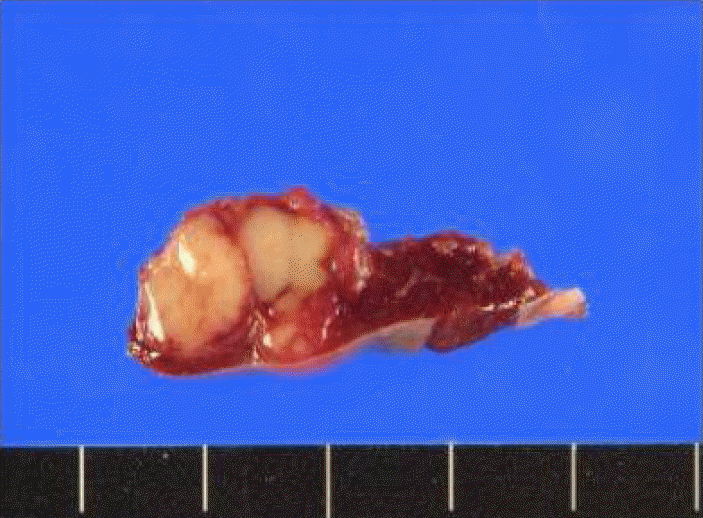
Laparoscopic splenectomy was performed, and the specimen showed a tumor 1.8 ├Ś 1.5 ├Ś 1.3 cm in size and light gray, and there was no evidence of capsular invasion (Fig. 4). Histological examination revealed a poorly differentiated carcinoma consistent with the features of primary nasal cavity cancer. There were metastases in two of seven lymph nodes. The patient was discharged 7 days after the operation. He has been on regular follow up with no clinical evidence of disease for 5 months since the operation.
With the improvement of loco-regional control in head and neck cancer, the incidence of distant metastatic disease in head and neck cancer appears to be rising. Pulmonary metastases are the most frequent, accounting for 66% of distant metastases. Other metastatic sites include the bone (22%), liver (10%), skin, mediastinum and bone marrow [4]. Once distant metastases have occurred, long-term survival is generally poor. The time interval between the diagnosis of distant metastases and death is less than 2 years in more than 90% of patients [4].
Although the prevalence of splenic metastases seems to increase with the improvement of medical imaging techniques, it remains uncommon [1,5]. Explanations proposed for the relative paucity of splenic metastasis have included (1) the sharp angle made by the splenic artery, which makes it difficult for tumor emboli to enter the spleen, (2) the absence of afferent lymphatics to bring the metastatic tumor to the spleen, and (3) antitumor activity due to a high concentration of lymphoid tissue in the spleen [1]. An autopsy of patients who died of head and neck cancer showed that, of the 832 patients autopsied, 387 were found to have histologically confirmed distant metastases at one or more sites, and 9% of them (35 patients) had splenic metastasis [5]. Only one case report to date has shown a solitary splenic metastasis from head and neck cancer [6].
This case suggests that splenic metastasis, although rare, may occur with successfully treated head and neck cancer. In the present case, the lesion in the spleen was an isolated metastasis in a locoregionally controlled nasal cavity cancer, and the metastasis occurred after ~7 months of a disease-free interval. Patients with recurrent or metastatic disease, who are not surgical or radiation therapy candidates, are usually offered palliative options, and systemic chemotherapy has become the standard of care in patients with recurrent or metastatic squamous cell carcinoma of the head and neck (SCCHN) [7]. The present case underwent systemic treatment initially because the lesion in the spleen was confirmed to be a metastasis by biopsy.
Although the experience related to metastasectomy is limited in head and neck malignancies [4], one study reported the management outcome of 377 patients who had recurrent head and neck cancer after primary curative surgery. Of the 95 patients with distant metastasis, 54 had lung metastasis and 6 (11%) were salvaged surgically; 5 of them had lung cancer recurrence, with a mean survival of 18 months; and 1 (17%) was tumor free with a follow up of 100 months. The mean survival of patients without surgical salvage was 6 months [8]. Additionally, some case reports have shown long-term survival after splenectomy in solitary splenic metastases in other types of solid tumors. Kousyou et al. reported a case of solitary splenic metastasis from gastric cancer in a patient who survived for 40 months after splenectomy [9]. Okuyama et al. reported that the 1-year survival rate and median survival after treatment of splenic metastasis in colorectal cancer were 86.6% and 66 months, respectively [10]. In our case, because the patient was young with a good performance status, local treatment for the splenic lesion was considered, and splenectomy was performed without complications.
Distant metastasis in head and neck cancer remains the major cause of mortality and treatment failure, despite better loco-regional control of the disease; therefore, it is crucial to evaluate the metastasis. Although rare, splenic metastasis of head and neck cancer does occur and should be considered for local and systemic treatment.
Acknowledgements
The authors thank the members of Seoul National University Hospital multidisciplinary team for head and neck cancer.REFERENCES
1. Lam KY, Tang V. Metastatic tumors to the spleen: a 25-year clinicopathologic study. Arch Pathol Lab Med 2000;124:526ŌĆō530.


2. Comp├®rat E, Bardier-Dupas A, Camparo P, Capron F, Charlotte F. Splenic metastases: clinicopathologic presentation, differential diagnosis, and pathogenesis. Arch Pathol Lab Med 2007;131:965ŌĆō969.


3. Vyas SJ, Chitale AR, Deshpande RK. Late splenic metastasis after curative resection for oesophageal carcinoma. Eur J Cardiothorac Surg 2002;22:1011ŌĆō1013.


4. Ferlito A, Shaha AR, Silver CE, Rinaldo A, Mondin V. Incidence and sites of distant metastases from head and neck cancer. ORL J Otorhinolaryngol Relat Spec 2001;63:202ŌĆō207.


5. Kotwall C, Sako K, Razack MS, Rao U, Bakamjian V, Shedd DP. Metastatic patterns in squamous cell cancer of the head and neck. Am J Surg 1987;154:439ŌĆō442.


6. Raval MV, Zemon H, Kumar SS, Brody FJ. Laparoscopic splenectomy for metastatic squamous cell cancer of the neck. J Laparoendosc Adv Surg Tech A 2005;15:383ŌĆō386.


7. Cohen EE, Lingen MW, Vokes EE. The expanding role of systemic therapy in head and neck cancer. J Clin Oncol 2004;22:1743ŌĆō1752.


8. Wong LY, Wei WI, Lam LK, Yuen AP. Salvage of recurrent head and neck squamous cell carcinoma after primary curative surgery. Head Neck 2003;25:953ŌĆō959.


A baseline examination. (A) Whole-body FDG PET at baseline shows intense uptake in the left nasal cavity primary mass. (B) Neck CT at baseline shows multiple enlarged cervical lymph nodes greater than 2 cm in diameter in the left level IB and II, and a left inferior nasal meatus mass.
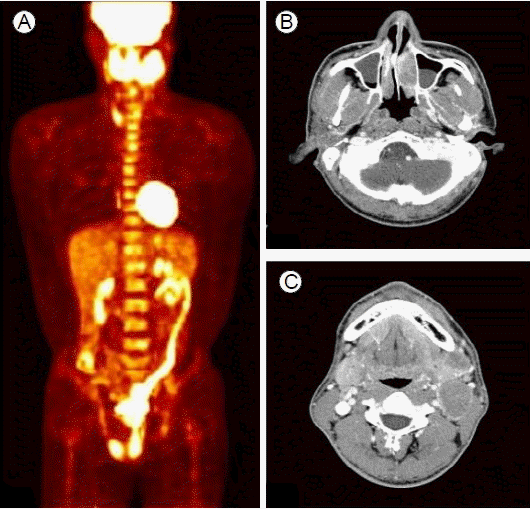
Figure┬Ā1.
Post-treatment examination. (A and B) Whole-body FDG-PET/CT after induction chemotherapy and operation shows no uptake in sites positive at baseline but shows intense uptake in the spleen. (C) Abdominal CT demonstrates a 2.5 cm slowly enhancing mass in the spleen without any notable findings in other organs.
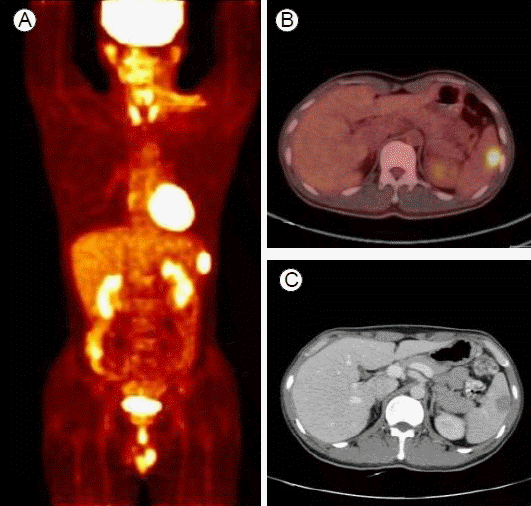
Figure┬Ā2.
Photomicrographs of the nasal cavity (A and C) and spleen biopsies (B and D). (A) The nasal cavity biopsy shows islands of tumor cells (hematoxylin and eosin staining, ├Ś 400). (C) The tumor cells are positive for Epstein-Barr virus by in situ hybridization (EBV-ISH) (├Ś 400). (B) A spleen biopsy shows a similar cancer cell nest in a fibrotic stroma (hematoxylin and eosin staining, ├Ś 200). (D) The tumor cells are also positive by EBV-ISH (├Ś 200).
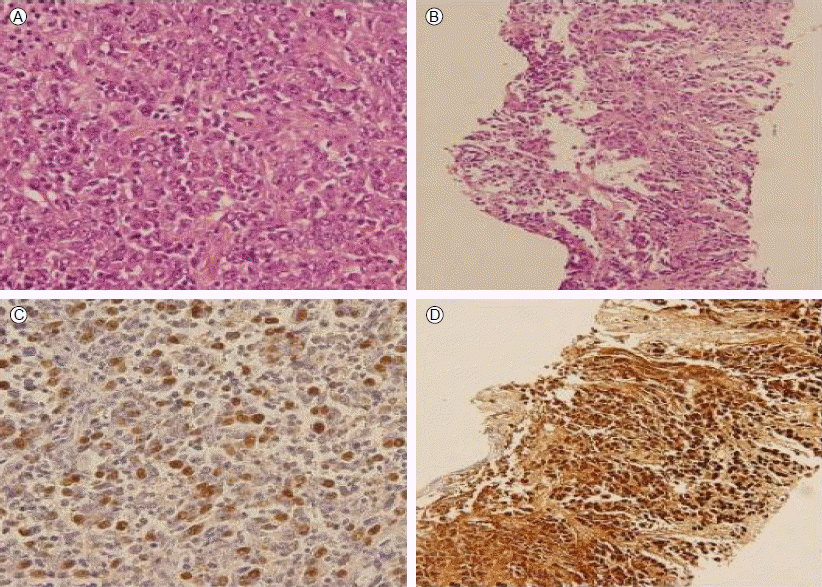
Figure┬Ā3.
-
METRICS

-
- 1 Crossref
- 0 Scopus
- 8,563 View
- 82 Download



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print



