INTRODUCTION
The radial artery has become the most common access site for coronary angiography and percutaneous coronary intervention (PCI) since transradial intervention results in fewer local vascular complications than transfemoral intervention [1]. This procedure rarely results in complications, improves patient comfort, and reduces the duration of hospitalization [2]. Despite the fact that complications are rare, radial artery perforation can result in compartment syndrome and acute hand ischemia [3]. The aim of this study was to share our experience in managing iatrogenic radial artery perforation.
CASE REPORT
A 69-year-old male was hospitalized for coronary intervention after evaluation by computed tomography (CT) revealed critical stenosis of the distal left circumflex artery (LCX).
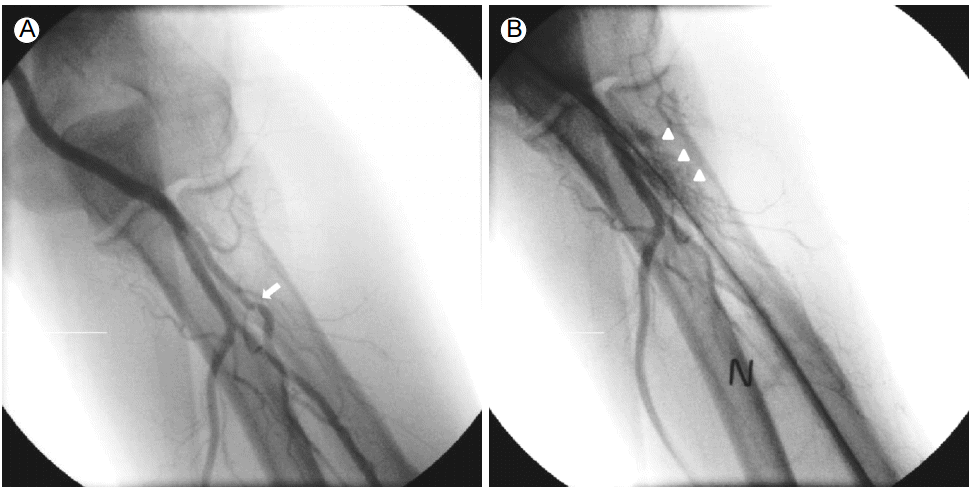
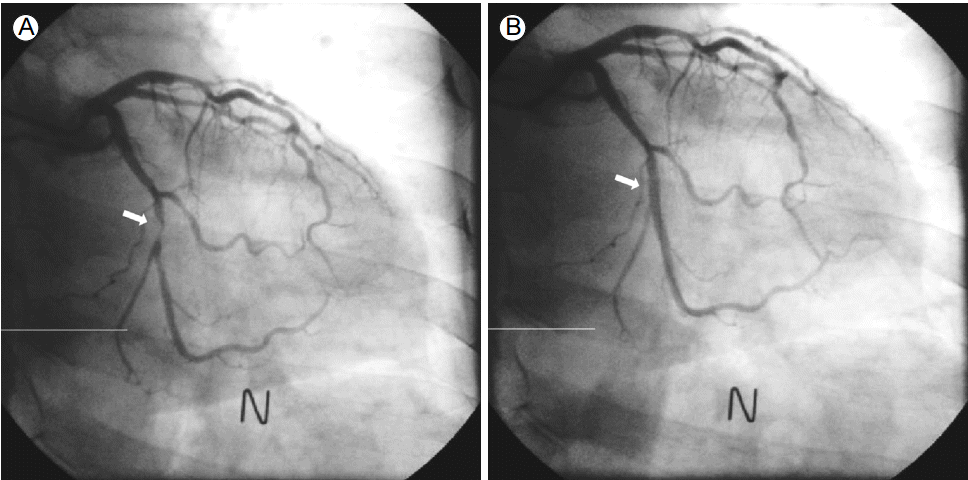
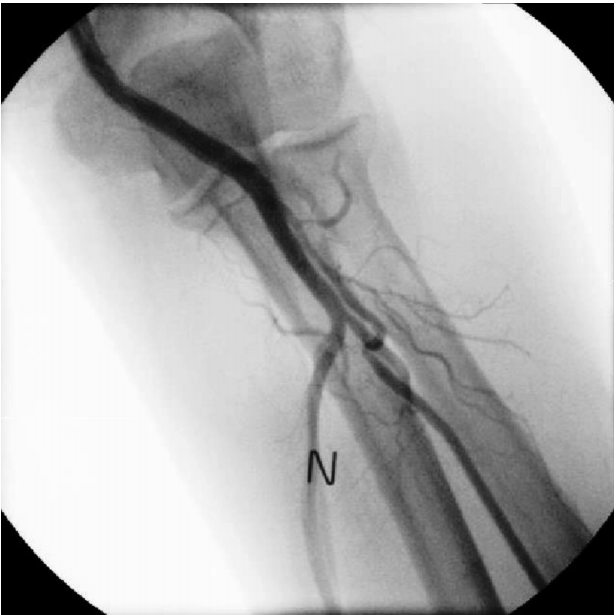
The patient underwent coronary angiography via the left radial route with a 6 French (Fr) sheath (Terumo Corp., Tokyo, Japan) inserted using standard techniques. The left radial angiography showed a minor degree radial artery spasm (Fig. 1A). After injecting 200 Ојg of nitroglycerin via the radial artery, coronary angiography was successfully performed with 5 Fr JL4 and JR4 diagnostic catheters. The distal LCX lesion was similar to the lesion revealed by the coronary CT scan (Fig. 2A); therefore, PCI was deemed the best treatment option. During insertion of a 6 Fr extra back-up (EBU) guiding catheter (Medtronic, Dublin, Ireland) over a 0.035-inch standard guidewire, the catheter encountered resistance and the patient complained of pain in the left forearm. After removing the 6 Fr EBU guiding catheter, radial angiography was performed by injecting diluted contrast agent through the side port of the sheath. The contrast agent revealed perforation and extravasation of contrast agent into the surrounding tissue (Fig. 1B). A 5 Fr EBU was able to pass the perforated segment over the remaining 0.035-inch standard guidewire. PCI was performed successfully with balloon angioplasty and a 2.75 X 18-mm stent (Resolute integrity, Medtronic, Dublin, Ireland) (Fig. 2B). After removing the guiding catheter, radial angiography was performed via the sheathвҖҷs side port. The procedure showed that the perforation was sealed and that there was no contrast agent extravasation (Fig. 3).
The patient was discharged after 48 hours without any local vascular complications, with a patent radial pulse, and no local hematoma.
DISCUSSION
The transradial approach is more popular due to decreased vascular complications and increased patient comfort [4]. The benefits of the transradial approach include a lower incidence of complications, earlier ambulation, same-day or next-day discharge, and a reduced cost of long-term hospitalization [2]. Despite its advantages, the transradial approach can result in significant complications, including local hematoma, radial artery obstruction, radial artery perforation, and hand ischemia. Radial artery perforation has been reported in about 1% of patients undergoing a transradial procedure. In the past, perforations have been treated by manual compression of the forearm or inflation of a balloon catheter across the perforated segment [5]. Once this complication occurs, the physician must switch to a contralateral radial or femoral approach to complete the procedure. This ultimately leads to an increase in both total procedure time and patient hospital stay. However, in this study, successful PCI was performed using the radial artery after perforation by downsizing the catheter and rewiring the perforated segment with a 0.014- or 0.021-inch PCI guidewire [6]. Using a smaller guiding catheter over the affected segment and a 0.035-inch guidewire for the rest enabled the procedure to continue without switching to another site. Since the guiding catheter itself worked as a hemostatic device, the perforation was sealed without further intervention. After successful completion of PCI, a radial angiogram was performed to check the hemostatic status of the perforated segment.
This case shows that simple installation of a smaller guiding catheter can seal perforations in the radial artery and prevent the physician from having to move to an alternate site.
In summary, radial artery perforation is one of the major complications of transradial PCI. By installing a small guiding catheter, the radial artery perforation was managed, and PCI was performed successfully using the same route. This case verifies that simple installation of a smaller guiding catheter can manage radial artery perforation during PCI.



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print






